

|
Author(s)
Wayne Naylor
|
Contents
|
|
Published:
July
2002
Last updated: Feb 2002 Revision: 1.0 |
Keywords: fungating wounds; symptom self-assessment; palliative care; patient-centred care plan; assessment tool.
Accurate assessment of symptoms is vital to provide correct treatment, evaluate effectiveness of interventions and gain an insight into patients' quality of life.
Assessment of fungating wounds should establish a patient's psychological and social state as well as local wound factors.
Patient ratings are generally considered the 'gold standard' for symptom reporting; self-reporting can be problematic for the very ill patient with advanced cancer.
The WoSSAC has been designed to measure the severity of symptoms and problems associated with fungating wounds, as well as the impact they have on the patient's life. The results of the assessment may be used to develop a patient centred care plan.
Fungating wounds are a significant problem for both patients and healthcare professionals. Not only do they signify progressive and life threatening disease, but they also significantly affect patients' quality of life by causing unpleasant and difficult to manage symptoms (see Part 1). Symptom control and appropriate psychosocial support are the main treatment goals aimed at improving quality of life. Accurate assessment is the cornerstone of effective symptom management and self-reporting by the patient may be considered to be the most appropriate method.
In Part 2 the development of a new symptom self-assessment tool, the Wound Symptoms Self-Assessment Chart (WoSSAC), is described. This tool allows patients to rate the severity of symptoms and problems they are experiencing, together with the level of interference they have on their daily lives. A pilot study is currently being conducted to assess the content validity of the WoSSAC.
The assessment of fungating wounds is an extremely important aspect of care. It should involve a holistic approach and include information on the patient's psychological and social state as well as local wound factors [1], [2], [3]. Collier [2] suggests that this may be achieved using a nursing model and recommends Roper, Logan and Tierney's 'Activities of Daily Living'.
The literature on fungating wounds indicates that the management of symptoms should be patient-focused. Grocott [4] suggests that management should be guided by problems identified by the patient, combined with the clinical concerns of health professionals. Other authors support this view, stating that symptom management priorities should be based on those problems identified by the patient as being the most troublesome [3], [5], [6], while Price considers the main aim of management to be an improvement in a patient's quality of life (QoL) [7].
It is vital that a consistent and reliable method of symptom assessment is used, as the information gained may be used to monitor the efficacy of treatment, side effects of treatment or to provide an insight into the patient's QoL [8]. This type of evaluation is of particular importance for the patient in the palliative care setting where curing disease is no longer possible and improving or maintaining QoL is the goal [9], [10], [11]. In order to reliably identify and rate symptoms it is useful to have a structured framework of assessment. Sarna [12], in a study involving patients with lung cancer, found that the use of a structured nursing assessment to evaluate symptom distress forestalled an increase in symptom distress over time. In this study, patients were given three self-report scales and one objective assessment. This type of structured assessment may produce better symptom relief by providing the necessary information for informed and personalised interventions [12].
The literature on chronic wound assessment offers some useful guidance which can be applied to the assessment of fungating wounds:
Accurate assessment is vital to provide correct treatment and evaluate the effectiveness of treatment approaches [13], [14], [15], [16], [17].
Wound assessment must never occur in isolation; instead a holistic approach that takes account of the whole person must always be taken [13], [14], [16], [18], [19], [20].
The use of documentation to assist in the assessment process is widely advocated to ensure that all relevant parameters are covered and to fulfil legal and professional requirements [13], [14], [15], [16], [21], [22], [23]. Current assessment focuses on documenting local wound characteristics only and the patient's QoL is an aspect of wound assessment and management that is often neglected [19], [24].
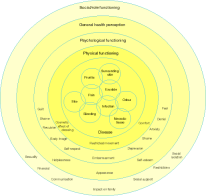
Figure 1 provides a conceptual model illustrating the potential impact of a malignant fungating wound on a patient's quality of life. The model is based on a framework proposed by Ware [25], and explores the interrelationships between wound symptoms/problems and their effect on different aspects of health and functioning. This framework moves beyond the immediate impact of disease to explore its effect on the patient's wider psychosocial environment [26]. Central to the model is the disease itself, with the initial impact on the patient's physiology. Therefore the central area of the model shows the wound-related symptoms and the interactions between these different symptoms. The effect then spreads outwards in concentric circles to physical functioning, psychological functioning, general health perception and social and role functioning. The objective of developing this model was to identify and visualise the relationships between the different aspects of fungating wounds and how these impact on other areas of health. The literature suggests that the psychosocial problems experienced by patients with fungating wounds are directly related to their symptoms and this model supports these findings. This conceptual model highlights the far-reaching consequences of living with a fungating wound and forms the basis of the patient assessment tool described below.
Following a literature review, a list of properties considered essential for an assessment tool for fungating wounds was developed (Table 1). These are based on the criteria proposed by Flanagan [14] for selecting an assessment instrument.
| The tool must: |
| Be easily understood by the healthcare professionals who may use it |
| Be easily understood and completed by the patient |
| Incorporate potential symptoms and problems that may be encountered by patients with a fungating wound |
| Be able to identify the symptoms and problems of most concern to the patient in relation to their wound |
| Provide a measure of the effect of symptoms and problems on the patient's QoL |
| Provide accurate assessment information that will guide management of the patient's wound |
| Be sensitive enough to measure change in symptoms |
| Be reliable and valid for use with patients who have fungating wounds |
Patient ratings are generally considered the 'gold standard' for symptom reporting [9]. However, for the very ill patient with advanced cancer, self-reporting can be a problem, especially if the patient has any cognitive impairment or communication difficulties, when self-reporting may become unrealistic [10], [27]. Difficulty may also occur if the patient is experiencing severe symptom distress or completing the tool is too physically or emotionally demanding [27]. However, it is at this point, when the patient is most unwell, that accurate assessment is so important [28]. Therefore self-assessment tools need to be brief, reliable and easily administered.
For this self-assessment tool a questionnaire format was chosen, as it provides a structured method of obtaining factual information and has a high degree of consistency for descriptive or comparative data [29]. This type of information is necessary for the development of an individualised management plan, as well as the ongoing evaluation of symptom and problem management strategies. Because questionnaires are standardised and structured they can provide reliable assessments over time and between patients [30].
A six-stage process for developing a questionnaire was adopted to establish the content and format of the assessment tool. This included item selection, item reduction, questionnaire format, pre-testing, reliability, and validity [31]. The new tool's working title is the Wound Symptoms Self-Assessment Chart or WoSSAC.
Items were selected that could potentially be incorporated into the tool. This included all the symptoms and problems identified from the literature on fungating wounds (Table 2) [1], [2], [3], [4], [6], [7], [32], [33], [34], [35], [36], [37], [38], [39], [40], [41], [42], [43], [44] .
| Wound | Psychosocial |
| Bleeding | Body image |
| Colour/condition of the wound bed | Communication difficulties |
| Comfort of dressings | Cosmetic effect of dressing |
| Devitalised tissue | Denial |
| Exudate | Depression |
| Frequency of dressing changes | Embarrassment |
| Infection | Fear |
| Location | Guilt |
| Odour | Impact on family |
| Pain | Information needs |
| Pain related to dressing changes | Restrictions due to dressing changes |
| Pruritis | Revulsion/disgust |
| Size/shape | Self-respect/self-esteem |
| Surrounding skin | Sexuality |
| Tunnelling/undermining | Shame |
| Social isolation | |
| Social support/resources |
The large number of items identified needed to be reduced to allow for easy and quick self-assessment. Some items were felt not to be appropriate, as patients would not be able to assess them easily or appropriately (e.g. physical aspects of the wound). At present a pilot study is being conducted with the aim of further reducing the number of items and evaluating content validity based on patient feedback. The items currently under review for inclusion in the WoSSAC include:
Pain from the wound
Pain related to dressing changes
Fluid (exudate) leakage from dressing
Bleeding from the wound
Smell (odour) from wound
Itching (pruritis) of the wound or surrounding skin
Comfort of dressing
Effect of dressings on looks (cosmetic effect of dressing)
Effect of wound on appearance (body image)
Effect of wound on mood (depression)
Effect of wound on feelings about self (self-esteem)
Effect of wound on social interaction (social isolation)
Restrictions due to dressing changes
Amount of social support
Information about wound
Feeling embarrassed about wound
Feeling ashamed about wound
Feeling guilty about wound
Effect of wound on relationship with partner
Effect of wound on family
Effect of wound on desire to go out
A self-report questionnaire must be easily read and understood by patients who, in some cases, may have advanced or terminal illness and it is important that the layout, wording and length is appropriate to this patient group. As this tool is intended to measure symptom distress, it was decided to evaluate both severity and interference with daily life of each symptom or problem. Patients are asked to rate both parameters for the previous seven days. Each item consists of two parts: a lead-in question (or stem) and a response set [45].
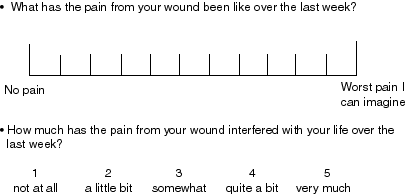
A visual analogue scale (VAS) was chosen for the response set to questions on severity (Figure 2). The VAS has been used to measure mood, anxiety, alertness, attitudes, functional abilities and severity of clinical symptoms, in particular pain [29] [45], [46]. A number of studies have evaluated various presentations of the VAS, such as longer lines, vertical presentation, dividing the line into segments and adding descriptors at various points along the line. The 100 millimetre, horizontal presentation where the patient is asked to place a mark on the line at the point that best describes their symptom appears to be the most effective [46].
For questions on the level of interference, a five-point Likert-type scale was used (Figure 2). This consists of a five-point numerical scale with declarative statements at each of the points. This type of scale is commonly used to determine opinion or attitude. Patients are asked to choose a number that best describes their current opinion [29]. This is an ordinal scale and there is no equal distance implied between each of the statements. They are, however, ranked in a hierarchical order to suggest that 'A little bit' is worse than 'Not at all' but better than 'Somewhat', and so on (see Appendix A).
The WoSSAC is intended to be used for multiple assessments over time. It will therefore need to incorporate an ongoing record of assessments to enable evaluation of any interventions. A 'Symptom Evaluation Grid' was developed, modelled on the Symptom Assessment Graph from the Edmonton Symptom Assessment System [47]. The Symptom Evaluation Grid records the severity and interference scores for each item for several assessments over a period of time. The severity is calculated by counting the divisions on the VAS and recording this number, to the nearest division, from the left-hand side ('best' side) to the patient's mark. This measurement is then transferred, as a score out of ten, to the grid. This part of the grid has a column that is divided into ten segments with one segment corresponding to one division on the VAS. Segments are coloured in according to the score, producing a visual graph of a patient's progress towards symptom/problem management goals. Underneath the column is a space to record the level of interference, which is simply the numerical score from the Likert scale (see see Appendix B).
Pre-testing or piloting of the tool is currently underway. Ten patients will be asked to examine each item and decide whether it applies to them or not and how easy each question is to understand. Patients will also be asked whether they feel any items are inappropriate. It is hoped that this method of content analysis will introduce the patient's view of what needs to be included in the chart. It is also planned to ask an expert panel to rate the content of the WoSSAC as part of the content validation process. The information gained from this part of the study will be used to evaluate content validity, or comprehensiveness, of the WoSSAC.
The final stages of the WoSSAC development will take place during a clinical study. Reliability relates to an instrument's ability to produce consistent results across patients, time or observers and validity is described as 'the extent to which a test measures what it is supposed to measure' [29], [45], [46]. Since the WoSSAC has a questionnaire format with a fixed structure and content it can be assumed to be reliable, and as a self-report tool, the reliability of the observer, or rater, will be consistent. However, problems may occur if the patient is too ill to complete the questionnaire and an alternative assessor, such as the patient's relative, has to complete it. The WoSSAC is primarily designed for individual patient assessments and to inform healthcare professionals about patients' immediate concerns. It is not designed for research purposes or to produce data for comparison between patients, therefore it could be argued that reliability across patients might not be essential [11]. However, with the current paucity of original research into the management of fungating wounds, the WoSSAC may provide a means of monitoring care over time and could be used to evaluate the efficacy of different treatment strategies.
At present, there is no valid and reliable method of self-assessment to assist in the evaluation of symptoms and problems related specifically to fungating wounds. One tool that has been utilised in the research setting for assessment by healtcare professionals is the TELER system of note-making [48], [49]. The TELER system comprises indicators, which track progress towards or away from a specific treatment goal [50]. It has been suggested that this system of note-making allows clinicians to view, 'at a glance', trends in patient problems and how they are related to the treatment or care given [51]. The TELER system does not lend itself to self-assessment by the patient and relies on clinicians to record information. This may introduce bias. The TELER system is available for a fee, which includes training and ongoing support.
The WoSSAC has been designed to measure the severity of symptoms and problems associated with fungating wounds, as well as the impact they have on the patient's life, from the patient's perspective. The results of this assessment can be used to develop a patient-centred care plan. The Symptom Evaluation Grid will allow for monitoring and comparison of patient symptoms and problems over time, as well as an assessment of the effectiveness of symptom management strategies. It is intended that the WoSSAC be used for any patient who has a fungating wound, whether they are in an advanced stage of their illness or have localised disease. The current pilot study of the WoSSAC will provide valuable data on its content validity, as well as the appropriateness and effectiveness of the questionnaire design. It will also supply useful information for the future development and implementation of this type of symptom assessment.
1. Haisfield-Wolfe ME, Rund C. Malignant cutaneous wounds: a management protocol. Ostomy Wound Manage 1997; 43(1): 56-60, 62, 64-6.
2. Collier M. The assessment of patients with malignant fungating wounds - a holistic approach: Part 2. Nurs Times 1997; 93(44): suppl 1-4.
3. Pudner R. The management of patients with a fungating or malignant wound. J Community Nursing (online) 1998; 12(9)Available from URL: http://www.jcn.co.uk/backiss.asp?YearNum=1998&MonthNum=09&ArticleID=82 [Accessed 18 February 2000].
4. Grocott P. Assessment of fungating malignant wounds. J Wound Care 1995; 4(7): 333-6.
5. Collier M. The assessment of patients with malignant fungating wounds - a holistic approach: Part 1. Nurs Times 1997; 93(44): suppl 1-4.
6. Jones M, Davey J, Champion A. Dressing wounds. Nurs Standard 1998; 12(39): 47-52.
7. Price E. Wound care. The stigma of smell. Nurs Times 1996; 92(20): 70-2.
8. Newell S, Sanson-Fisher RW, Girgis A, Bonaventura A. How well do medical oncologists' perceptions reflect their patients' reported physical and psychosocial problems? Data from a survey of five oncologists. Cancer 1998; 83(8): 1640-51.
9. Nekolaichuk CL, Bruera E, Spachynski K, MacEachern T, Hanson J, Maguire TO. A comparison of patient and proxy symptom assessments in advanced cancer patients. Palliat Med 1999; 13(4): 311-23.
10. Lobchuk MM, Kristjanson L, Degner L, Blood P, Sloan JA. Perceptions of symptom distress in lung cancer patients: I. Congruence between patients and primary family caregivers. J Pain Symptom Manage 1997; 14(3): 136-46.
11. Rathbone GV, Horsley S, Goacher J. A self-evaluated assessment suitable for seriously ill hospice patients. Palliat Med 1994; 8(1): 29-34.
12. Sarna L. Effectiveness of structured nursing assessment of symptom distress in advanced lung cancer. Oncol Nurs Forum 1998; 25(6): 1041-8.
13. Miller M. Nursing assessment of patients with non-acute wounds. Br J Nurs 1999; 8(1): 10-6.
14. Flanagan M. A practical framework for wound assessment. 2: Methods. Br J Nurs 1999; 6(1): 6, 8-11.
15. Moore Z. Wound care: module 2; Part 6: Local wound assessment. World Ir Nurs 1997; 5(6): 15-6.
16. Benbow M. Parameters of wound assessment. Br J Nurs 1995; 4(11): 647-8, 650-1.
17. Miller P, Powell D. Developing wound evaluation tools. Nurs Stand 1995; 9(40): 25-7.
18. Casey G. Assessing wounds. Nurs N Z 1997; 3(5): 26.
19. Moore Z. Wound care: module 2; Part 5: Holistic patient assessment in wound care. World Ir Nurs 1997; 5(5): 15-6.
20. Miller M. Best practice in wound assessment. Community Nurse 1996; 2(3): 41-2, 44, 47.
21. Bachand PM, McNicholas ME. Creating a wound assessment chart. Advances in Wound Care 1999; 12: 426-29.
22. Sterling C. Methods of wound assessment documentation: a study. Nurs Stand 1996; 11(10): 38-41.
23. Collier M. Assessing a wound (continuing education credit). Nurs Stand 1994; 8(49 Suppl Nu): 3-8; quiz 11-3.
24. Thomas S, Fear M, Humphreys J. Assessment of patients with chronic wounds. J Wound Care 1994; 3(3): 151-54.
25. Ware JE. Conceptualizing disease impact and treatment outcomes. Cancer 1984; 53: 2316-23.
26. Clinch JJ, Dudgeon D, Schipper H. Quality of life assessment in palliative care In: Doyle D, Hanks GWC, MacDonald N, editors. Oxford Textbook of Palliative Medicine (2nd edition). Oxford: Oxford University Press, 1998; 83-94.
27. Sneeuw KCA, Aaronson NK, Sprangers MAG, et al. Evaluating the quality of life of cancer patients: assessments by patients, significant others, physicians and nurses. Br J Cancer 1999; 81(1): 87-94.
28. Grassi L, Indelli M, Maltoni M, et al. Quality of life of homebound patients with advanced cancer: assessments by patients, family members and oncologists. J Psychosocial Oncology 1996; 14(3): 31-45.
29. Waltz CF, Strickland OL, Lenz ER. Measurement in Nursing Research (2nd edition). Philadelphia: FA Davis Company, 1991.
30. Parahoo K. Nursing Research Principles, Process and Issues. Basingstoke: Macmillan Press, 1997.
31. Gyatt GH, Bombardier C, Tugwell PX. Measuring disease-specific quality of life in clinical trials. CMAJ 1986; 134: 889-95.
32. Haisfield-Wolfe ME, Baxendale-Cox LM. Staging of malignant cutaneous wounds: a pilot study. Oncol Nurs Forum 1999; 26(6): 1055-64.
33. Grocott P. The management of fungating wounds. J Wound Care 1999; 8(5): 232-4.
34. Fairbairn P. A challenge that requires further research: management of fungating breast lesions. J Wound Care 1994; 9(4): 272-77.
35. Hallett A. Fungating wounds. Nurs Times 1995; 91(47): 81-85.
36. Grocott P. The palliative management of fungating malignant wounds. J Wound Care 1995; 4(5): 240-2.
37. Young T. The challenge of managing fungating wounds. Community Nurse 1997; 3(9): 41-4.
38. Woodhouse P. Wound care nursing. Managing a breast wound. Nurs Times 1992; 88(12): 72-5.
39. Grocott P. Wound care - practical changes. Nurs Times 1993; 89(7): 64, 66, 68 passim.
40. Boardman M, Mellor K, Neville B. Treating a patient with a heavily exuding malodorous fungating ulcer. J Wound Care 1993; 2(2): 74-76.
41. Davis V. Goal-setting aids care. Nurs Times 1995; 91(39): 72-75.
42. Carville K. Caring for cancerous wounds in the community. J Wound Care 1995; 4(2): 66-8.
43. Saunders S. Mutual support. Nurs Times 1997; 93(32): 76-82.
44. Bycroft L. Care of a handicapped woman with metastatic breast cancer. Br J Nurs 1994; 3(3): 126-8, 130-3.
45. Burns N, Grove SK. The Practice of Nursing Research. Conduct, critique and utilisation (3rd edition). Philadelphia: WB Saunders, 1997.
46. McDowell I, Newell C. Measuring Health: A guide to rating scales and questionnaires (2nd edition). Oxford: Oxford University Press, 1996.
47. Bruera E, Kuehn N, Miller MJ, Selmser P, Macmillan K. The Edmonton Symptom Assessment System (ESAS): a simple method for the assessment of palliative care patients. J Palliat Care 1991; 7(2): 6-9.
48. Grocott P. Developing a tool for researching fungating wounds. World Wide Wounds 2001; Available from URL: http://www.worldwidewounds.com/2001/july/Grocott/Fungating-Wounds.html [Accessed 4 July 2002].
49. Grocott P. Evaluation of a tool used to assess the management of fungating wounds. J Wound Care 1997; 6(9): 421-26.
50. Grocott P. Exudate management in fungating wounds. J Wound Care 1998; 7(9): 445-48.
51. le Roux AA. Summary of TELER (online). 2001; Available from URL: http://www.teler.com/teler.htm [Accessed 7 July 2002].
These questions are available as a PDF or Microsoft Word file.
The WoSSAC symptom evaluation grid is available as a
PDF or
Microsoft Word
file.