

|
Author(s)
Jenny Wall
Theresa Colley
|
Contents
|
|
Published:
Apr 2004
Last updated: Apr 2004 Revision: 1.0 |
Keywords: prevention; pressure ulcers; expert patient; risk assessment; wheelchair users.
The prevalence of pressure ulcers among permanent wheelchair users remains high. While many risk factors for pressure ulcer development in this group have been identified only a minority of these have been evaluated scientifically and it is generally acknowledged that existing risk assessment tools are inadequate for predicting risk in seated persons who use a wheelchair for mobility.
A 2-year prospective study is underway to design a new self-administered pressure ulcer risk indicator to be used by non-ambulant wheelchair users and their carers in conjunction with professionals. This instrument will be designed as a result of triangulation of methods.
A systematic review of available evidence
Latest professional opinion
A qualitative study exploring the issues from the perspective of seated persons with a history of pressure ulcers (n=10) undertaken by one of the authors (JW)
A 2-year prospective study identifying key risk factors in a sample of 160 seated persons.
This paper offers an insight into the findings on the recruitment of the 160 individuals into the prospective study, which is currently collecting a large amount of data on the health, degree of disability and integrity of skin of all the participants. The paper offers an overview of the medical diagnosis, degree of physical disability, issues pertaining to continence and prevalence of pressure ulcers in this group on recruitment. Early findings suggest that the new risk indicator should include measures of degree of physical disability and ability to transfer as an integral part of self assessment and therefore prevention of pressure ulcers. The study was due for completion in the autumn of 2002. It is envisaged that early work on the development of the tool should be complete by the summer of 2003.
One of the many unique features about being human is that most of us are bipedal - able to sit or stand to carry out activity or functions. For those who are unable to stand or walk, for whatever reason, seating becomes the sole position which is adopted for the majority of the day. The numbers of persons seated for the purposes of mobility remains poorly understood. A report by the Royal College of Physicians [1] dating back to 1995 estimate there to be about 650,000 seated individuals in the UK, of which 500 000 were thought to have a permanent disability [2]. In 2001 one regional UK wheelchair service in the Midlands, serving a population of 559 000, estimated the number of clients in receipt of at least one wheelchair (many have two chairs: one electric, one manual) to be 10 500. Although it is difficult to speculate on the generalisability of the figures from this particular service they suggest that approximately 1.8% of the population of the UK may be in receipt of a wheelchair. The prevalence of pressure ulcers in seated persons is poorly understood. Figures range widely: Sugarman [3] suggested that up to half of all seated persons with complex impairments would develop a pressure ulcer at some time during their life time. Stockton [4] in a study of 48 seated persons reported a prevalence of 60%. Inam and Firth [5] reported a prevalence of 4.9% in a study of over 1000 community patients and more recently Stockton and Parker [6] reported an overall prevalence of up to 58%.
From the clinical experience of the authors of this paper, pressure ulcers are a frequent and distressing aspect of the management of persons with complex physical disability. Studies suggest the cost of pressure ulcers is high in both human and financial terms:'A pressure sore can cause pain, systemic illness, reduced self-esteem, altered body image and can sufficiently delay rehabilitation measures to preclude return to independence'[7].
Pressure ulcers can result in long hospital stays, surgery, and prolonged bed rest at home, an increase in secondary disabilities such as contractures from bed rest and in extreme cases death from septicaemia [7]. In a study by the first author it was found that ten regular wheelchair users with pressure ulcers spent 1231 days or 3.37 years in hospital for ongoing treatment of pressure ulcers [8]. A study by Inam and Firth [5] found the average time spent by a district nurse on the treatment of one pressure ulcer was 3.4 hours per week and on prevention was 1.3 hours per week.
The causes of pressure ulcers are well researched, and they are known to be the result of a complex set of interactions; for example pressure, friction, shear, nutritional status, mobility, incontinence and acute illness [9],[10],[11],[12] are known to be of particular importance. These factors can be usefully categorised as either intrinsic (those from within) or extrinsic (external factors)[13].
In patients who are permanently seated a major risk factor is that nearly half of the body's weight is supported by 8% of the seated area, namely the areas surrounding the ischial tuberosities [14],[15],[16]. The seated individual potentially exposes a small area of their anatomy to considerable forces. The area surrounding the ischial tuberosities is therefore particularly vulnerable to these pressures.
Several specific risk factors are well documented. Pelvic obliquity, when the pelvis is tipped at an angle, can lead to excessive weight being transferred to the sacral area [17]. This often occurs so weight is redistributed as if rolling backwards off the back of the ischial tuberosities. Prolonged sitting also causes postural changes, such as lumbar lordosis [18], which in turn contribute to the additional risk associated with the poor distribution of the body weight [19].
Much work has been undertaken to prevent pressure ulcers from occurring and it has long been a challenge to the individuals at risk, their carers, health professionals and indeed health organisations in the UK. Since the pioneering work of Doreen Norton [20] the nursing profession, as part of their duty of care [21], have included pressure ulcer risk assessment as an integral part of their role. At least ten risk assessment tools are well documented in the UK literature and over forty reported worldwide [9],[10],[11]. The research evidence on the sensitivity and specificity (the ability to predict accurately those who will and will not develop ulcers) of the tools and therefore their usefulness is inconclusive [9],[22],[23],[24],[25]. In addition current risk assessment tools are widely thought of as having ceiling effects (i.e. predicting all regular wheelchair users as high risk, when they are sometimes not) and therefore offer high sensitivity and poorer specificity to this group of persons. The existing tools allow for little discrimination between the wheelchair user with good upper body strength who is therefore able to move freely and the user with advanced disease or severe injury who is unable to move at all. Neurological symptoms (those which affect sitting ability such as degree of physical disability, poor trunk control, deficits in sensation or balance and the inability to distribute body weight evenly when seated) are not currently reflected in risk assessment tools.
Most people who use a wheelchair for the purposes of mobility rely on the 'eyes' of their carers, both formal and informal (relatives), for monitoring skin integrity and for early detection of problems. Stockton [4] found that 50% of 48 permanent wheelchair users reported that their ulcers commenced while in hospital and the other 50% reported that they occurred while at home. The overall conclusion of this study was the need for education for those at risk, although it was recognised that information alone may not alter behaviour and therefore potential risk. A recent study by Stockton and Parker [6] reported inadequate pressure-relieving activity on behalf of 136 participants in a survey exploring behaviour and pressure ulcer prevention. Barnes [26], as a result of a postal survey of 27 health professionals, identified three broad categories of risk elements from which educational strategies could be identified. These comprised education around healthy lifestyle, functional ability and physical characteristics such as continence and skin condition.
There are currently no published self-administered pressure ulcer risk assessment tools in the UK that have been designed and validated for this group of persons. There is a growing recognition of the importance of self assessment [27], [28], and therefore prevention, in the continued challenge of reducing this largely avoidable condition. The available knowledge on the circumstances that predispose some seated persons to develop serious pressure ulcers while others in similar circumstances never develop ulcers is poorly understood. It is with these challenges in mind that this study is exploring the circumstances leading to pressure ulcer development in this group. The overall aim of the study is to evaluate the circumstances that predispose some seated individuals to pressure ulcer development. It is hoped that the insights from this 2-year prospective study will contribute to the development of a useful self-administered risk assessment tool for this group of persons.
This study seeks to further explore and develop understanding into the issues that predispose seated persons to the development of pressure ulcers. A longer-term objective is that these findings will contribute to the design of a self-administered tool to be used by those at risk in conjunction with both formal and informal carers.
Participants were recruited to the study following an advertising campaign in hospital clinics, rehabilitation inpatient services, voluntary organisations, support groups for the disabled and word of mouth across two counties in the middle of England during 2001. Participants were sought who used a wheelchair for the purposes of mobility. It quickly transpired that a cut-off point for minimum use of a wheelchair was required as several persons, particularly those with chronic or progressive disabilities, used a wheelchair intermittently or even unpredictably. Therefore some participants were recruited who required a wheelchair for all mobility needs outside of their immediate home environment (an assumption being that they would be seated more than usual at home) or those who used a chair for a minimum of 2 consecutive hours daily in their home. Calculations for the number of volunteers required for the study were difficult to determine accurately as a result of the very variable figures on the incidence of pressure ulcers in this group of persons. The ability of this study to generalise any findings to the wider population of seated persons is partly dependent on the sample size. Following statistical advice a formal power calculation was not undertaken, with the assumption that a sample size of 200 would provide the study with appropriate information. The inclusion criteria for recruitment to the study were:
Persons aged 18-70 years who use a wheelchair for the purposes of mobility for a minimum of 2 consecutive hours daily and/or require a wheelchair for all mobility outside the immediate home environment
Persons who had access or ability to monitor the integrity of their own skin and/or a carer willing to undertake this role
Persons and carers (where appropriate) both willing and able to give informed consent or assent.
On recruitment baseline data were collected on the health, degree of disability and skin condition of all the volunteers. The study was designed to compare potential risk factors, for example the ability to lift the buttocks free of the chair with the predictive value of the Waterlow score [29] and the Braden score [30] and to seek a correlation with a measure of disability (the Barthel index [31]). These measures were all recorded on recruitment. Pressure ulcer classification was achieved when necessary using a widely used and well-validated classification scoring system [32](Figure 1). All those taking part in the study provided informed and written consent. Ethical approval was gained from the relevant ethics committees for the two hospital trusts to recruit participants from the geographic areas covered by those trusts.
The recruitment process was undertaken as a convenience sample. It was felt that attempts to recruit a representative sample of wheelchair users were not logistically possible because of financial and time constraints. Following a year of recruitment 160 seated persons had consented and been enrolled into the study. It is envisaged that this sample will provide insights and offer some generalisability to the wider population of seated persons.
As indicated in Table 1 some data were collected using newly designed three-point scales, as shown in Table 2. Examples of the scales used can be obtained from the first author. The reason for this is that it was important to collect data in a way that would be easily transferable to a self-administered format. As no such validated or reliable scales were available for use the design of these scales became a necessary part of the study objectives despite the disadvantages of not using a validated tool. In addition the scoring process needed to be easily understood and visualised by potential users of a new self-assessed risk tool. Volunteers and their carers were asked to score each of the questions for themselves, and advice was offered by the research nurse collecting the data on request. For example a degree of physical disability was measured as demonstrated in Table 2. Scores reflect the nearest description of the participants of themselves as assessed on the day of recruitment. All three-point scales were designed to reflect descriptive and numerical categorical scores that rose with severity or increased risk to facilitate limited analysis of the results for the purposes of this paper. Numerical categories of the descriptions was also useful to describe the scoring method during the recruitment process with the volunteers. However, no weighting of numerical scores is possible until the study is complete. All other data are being collected by direct questions or questionnaires and are being stored on a Microsoft Access database (version XP).
| Data categories | |
| Demographics | Degree of physical disability* |
| Medical history | Competence in transfers* |
| Nursing history | Degree of incontinence/wetness* |
| Details of carer(s) | Use of specialist seating* |
| Smoking history | Body weight outside the normal range* |
| Medications | Diet* |
| Waterlow score | Acute illness* |
| Barthel score | Altered muscle tone* |
| Braden score | Sensory impairment* |
| Detailed history of ulcers | Levels of knowledge (client and carer)* |
| Current ulcers | Self and professional judgement* Subjective measure of motivation* |
All data marked* were collected using newly designed 3-point scales
| Degree of physical disability as assessed by ability to life buttocks free of the chair | |
| Able to alter position by being able to lift buttocks free of the chair as needed (minimum every 2 hours) | Low risk: score 0 |
| Able to move buttocks from side to side or lean forwards to alter position and relieve pressure | Medium risk: score 1 |
| Unable to alter position without assistance | High risk: score 2 |
One hundred and sixty participants were recruited to the study, aged from 21-69 years (mean 48 years). The number of years for which participants had been immobile ranged from a period of time less that 1 year to 64 years (mean 12.3 years). Of the sample, 96 were female and 64 were male, 100 were residents of southern Derbyshire and 60 were residents of central Nottingham. The primary diagnosis (some had as many as six differing diagnoses) of the 160 participants fell into the categories shown in Table 3.
| Diagnosis | Frequency | % |
| Multiple sclerosis | 69 | 43.1 |
| Cerebral palsy | 24 | 15.0 |
| Cerebral vascular accident | 12 | 7.5 |
| Head injury | 9 | 5.6 |
| Friedreich's ataxia | 6 | 3.8 |
| Spina bifida | 6 | 3.8 |
| Spinal injury | 7 | 4.4 |
| Subarachnoid haemorrhage | 3 | 1.9 |
| Muscular dystrophy | 2 | 1.3 |
| Leg amputation | 2 | 1.3 |
| Other - progressive | 13 | 8.1 |
| Other - non-progressive | 7 | 4.4 |
| Total | 160 | 100.0 |
Figure 2 shows that 68 (42%) of the 160 persons recruited to the study were unable to move their buttocks at all when seated and Figure 3 shows that 79 (49%) required the help of two persons and/or a hoist for all transfers.
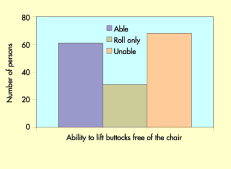
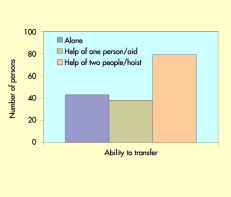
Thirty nine per cent or 64 persons had a history of pressure ulcers and, of those, eighteen persons reported current ulcers on the day of enrolment (Table 4).
| Site | Frequency | % |
| Sacrum | 9 | 50.0 |
| Buttock | 4 | 22.2 |
| Hip | 1 | 5.6 |
| Foot | 2 | 11.1 |
| Ankle | 2 | 11.1 |
| Total | 18 | 100.0 |
Participants reported where they were when they recalled their pressure ulcer(s) as commencing. Of these, 11% reported ulcers commencing while they were in hospital, 61% at home and the remainder as occurring while in a nursing home in receipt of respite care or permanent residence in a care establishment.
The recruitment of 160 seated persons offered an opportunity to take a 'snap shot' look at any emerging trends or differences between those with and without pressure ulcers. For this purpose the sample was divided into two sub-groups:
Group A: Those with no ulcers or history of pressure ulcers
Group B: Those with current ulcers or giving a history of pressure ulcers.
As Figure 4 and Figure 5 illustrate there is a skewed distribution in the number of years the participants had been seated. The majority of persons had been seated for 10 years or less (68% of group A and 63% of group B). The two groups do not appear to differ with respect to age, gender and years seated as presented in Table 5.
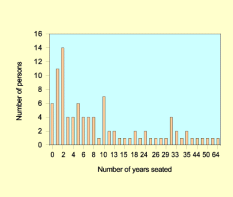
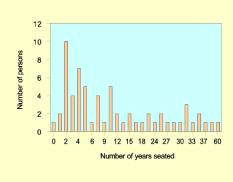
| Group A No history of ulcers n=96 | Group B Current or history of ulcers n=64 (18 current) | ||
| Age | Mean 48.3 years (SD=10.8) | Mean 47.2 years (SD=11.7) | |
| Gender | Male | 37 (39%) | 27 (42%) |
| Female | 59 (61%) | 37 (58%) | |
| Years seated* | Mean 12.1 years (SD=14) | Mean 12.8 years (SD=13) |
* Number of years seated for the purposes of mobility outside of the immediate home environment. SD = standard deviation
Further analysis revealed that participants with a progressive disability had been seated for a mean 7.39 years (standard deviation = 7.5 years) and those with a non-progressive condition demonstrated much greater variance (mean number of years seated 19.14 years; standard deviation = 16.8 years). No significant differences were obtained when comparing the mean classification of the ulcers reported by the two groups (Levene's test t= -0.222; degrees of freedom 156, p= 0.978).
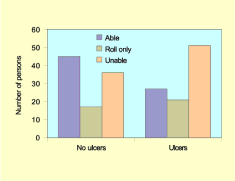
When comparing the two groups by degree of physical disability, as measured by ability to lift buttocks free of the seat and degree of assistance needed with transfer, some differing trends emerged. Analysis was undertaken using the scores as recorded for the purposes of this paper by the participants on the three-point scales.
As Figure 6 indicates, in the group without ulcers, 36.5% of the sample were unable to lift or transfer without the assistance of two persons or a hoist. This figure rose to 51.6% of persons in the group with ulcers. This finding was found not to be statistically significant when comparing the mean of the scores (Levene's test t = -2.432; degrees of freedom = 158; p=0.954).
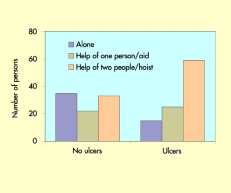
Similarly the difference in the ability to transfer demonstrated a similar trend (Figure 7). These figures were 42.7% (no ulcers) and 59.6% (current or with a history of ulcers). This finding was found to be statistically significant using comparison of mean scores (Levene's test t = 2.724, p = 0.05).
As part of the design of the evaluation study all volunteers had Waterlow, Braden and Barthel scores recorded on enrolment to the study. Once again this offered an opportunity to explore differences between the ulcers and no ulcers groups as illustrated in Table 6.
| Whole sample n=160 | Group A n=96 | Group B n=64 | |
| Waterlow score | 18.29 (SD=2.95) | 17.97 (SD=2.89) | 18.78 (SD=3.00) |
| Braden score | 15.43 (SD=2.75 | 15.84 (SD=2.78) | 14.80 (SD=2.6) |
| Barthel index | 7.17 (SD=4.38) | 8.07 (SD=4.41) | 5.83 SD=4.00) |
SD = standard deviation
The Waterlow and Braden scores were found to be negatively correlated (Spearman's rho = -0.491, p = 0.01; two tailed). The Barthel index was found to correlate with both the Waterlow (Spearman's rho = +0.462, p = 0.01) and the Braden score (Spearman's rho = - 0.702, p = 0.01). Measures of degree of physical disability and ability to transfer were found to be correlated to each other (Spearman's rho = 0.795, p = 0.01; one tailed) (Table 7).
| Whole sample n=160 | Group A No history of ulcers n=96 | Group B Current or history of ulcers n=64 (18 current) | ||
| Ability to lift buttocks free of the chair | Median | 1 | 1 | 2 |
| Mean | 1.04 (SD=0.89) | 0.91 (SD=0.90) | 1.25 (SD=0.85) | |
| Ability to transfer | Median | 1 | 1 | 2 |
| Mean | 1.25 (SD=0.84) | 1.08 (SD=0.87) | 1.43 (SD=0.75) |
SD = standard deviation
Analysis of mean differences for the correlated scores for ability to move buttocks and ability to transfer when comparing those with and without pressure ulcers revealed the following assuming unequal variance between the two groups.
No significance difference between mean Waterlow scores (Levene's test t= 1.702)
No significance difference between mean Braden scores (Levene's test t= 2.424)
The Barthel index score was lower (indicating greater physical disability) in the group with ulcers. However, this finding was not statistically significant by comparison of mean scores (Levene's test t= 3.335).
A positive correlation was demonstrated between scores for the ability to move the buttocks and the Barthel index. (Spearman's rho = -0.841, one tailed; p = 0.01), and between scores for the ability to transfer and the Barthel index (Spearman's rho = -0.768, one tailed; p =0.01).
Table 8 gives an overview of the findings regarding bladder management and wetness of the two groups on enrolment. Figures do not add to 100% because most volunteers scored more than once. For example individuals may have scored in the category of ISC (intermittent self-catheterisation) and the degree of wetness experienced.
| Group A No history of ulcers n=96 | Group B Reported ulcers ulcers n=64 | |
| Never wet | 50 (52.1%) | 29 (45.3%) |
| Occasionally wet (2/3 times weekly) | 19 (19.8%) | 19 (29.7%) |
| Frequently wet (<3 times weekly) | 27 (28.1%) | 16 (25%) |
| No catheter | 68 (70.8%) | 29 (45.3%) |
| Urethral catheter | 10 (10.4%) | 14 (21.9%) |
| Suprapubic catheter | 11 (11.5%) | 15 (23.4%) |
| Intermittent self-catheterisation (ISC) | 3 (3.1%) | 3 (4.7%) |
| Other | 4 (4.2%) | 3 (4.7%) |
It is interesting that over 45% of the ulcerated group had either a urethral or suprapubic catheter compared to 22% of the non-ulcers group. However, it is possible to speculate that catheterisation may form part of pressure ulcer management and that once inserted becomes a long-term treatment. Of note is that 47.9% of the non-ulcers group reported a degree of wetness compared to 54.7% of the ulcers group. Further analysis of this finding by comparison of the mean of the scores for both groups revealed no significance difference (Levene's test t = - 0.269). However, a linear relationship was found between experienced degree of wetness and degree of physical disability as measured by ability to lift buttocks (Spearman's rho = 0.247, one tailed; p = 0.01) and ability to transfer (Spearman's rho = 0.189, one tailed; p = 0.01). It is possible that this finding reflects the dual problems of restricted mobility in getting to the toilet as well as increasing possible dysfunction of the bladder as impairment increases.
The preliminary findings of this study are of interest as they demonstrate some measurable differences in a group of permanent wheelchair users in which almost 40% of the group had had pressure ulcers during the 2 years before data collection. Caution must be used in making inferences regarding prevalence of pressure ulcers from these findings. The sample was not random and it is possible that participants who had experienced or had current pressure ulcers were more motivated to volunteer for this study, which is reflected in the findings.
It has only been possible to present some of the initial findings from the vast amount of data collected. The findings presented are of particular interest to the authors and much work is required to fully describe and analyse all the findings from the data collected during 1 year on the 160 seated persons. However, it is encouraging that initial analysis suggests that inclusion of the degree of physical impairment as measured by ability to lift the buttocks free of the chair and ability to transfer demonstrated some validity when comparing the performance of these measures with the well-validated Braden scale and Barthel index. It is suggested that these measures of impairment could be included in self-administered risk assessment for this group of persons.
This study has been funded by the Multiple Sclerosis Trust and Mansfield District Primary Care Trust. The authors would like to thank Professor Chris Ward, University of Nottingham, Dr Lorraine Pinnington, University of Nottingham, and Dr Diane Playford, University College London (formerly University of Nottingham), for their help and support with this study.
1. Royal College of Physicians of London. The provision of wheelchairs and specialist seating. London: Royal College of Physicians Publications Unit, 1995.
2. Sanderson D, Place M, Wright D. Evaluation of the powered wheelchair and voucher scheme initiatives. York: York Health Economics Consortium, 2000 (www.doh.gov.uk/pdfs/yhec.pdf).
3. Sugarman B. Infection and pressure sores. Arch Phys Med Rehabil 1985; 66(3): 177-79.
4. Stockton L. Preventing pressure sores in wheelchair users. Nurs Standard 1994; 18(20): 54-56.
5. Inman C, Firth JR. Pressure sore prevalance in the community. Prof Nurs 1998; 13(7): 515-20.
6. Stockton L, Parker D. Pressure relief behaviour and the prevention of pressure ulcers in wheelchair users in the community. J Tissue Viability 2002; 12(3): 84-99.
7. Clay M. Pressure sore prevention in nursing homes. Nurs Stand 2000; 14(44): 45-50.
8. Wall J. Preventing pressure sores among wheelchair users. Prof Nurse 2000; 15(5): 321-24.
9. Hamilton F. An analysis of the literature pertaining to pressure sore risk assessment scales. J Clin Nurs 1992; 1: 185-93.
10. Johnson J. Pressure area risk assessment in a neurological setting. Br J Nurs 1994; 3(18): 926-8, 930-1, 933-5.
11. Anon. Effective Healthcare Bulletin. University of Leeds: Nuffield Institute for Health, 1995; 2(1): 1-16.
12. Yarkony GM. Pressure ulcers: a review. Arch Phys Med Rehabil 1994; 75(8): 908-17.
13. Dealey C. The size of the pressure sore problem in a teaching hospital. J Adv Nurs 1991; 16(6): 663-70.
14. Crow R. Wound care. The challenge of pressure sores. Nurs Times 1988; 84(38): 68-73.
15. Sumiya T, Kawamura K, Tokuhiro A, Takechi H, Ogata H. A survey of wheelchair use by paraplegic individuals in Japan. Part 1: Characteristics of wheelchair cushions. Spinal Cord 1997; 35(9): 590-94.
16. Gebhardt K, Bliss MR. Preventing pressure sores in ortopaedic patients - is prolonged chair nursing detrimental? J Tissue Viability 1994; 4(2): 51-54.
17. Zacharkow D. Posture, sitting, standing, chair design and exercise. Springfield IL: CC Thomas, 1998.
18. Jay E. How different constant low-pressure support surfaces address pressure and shearing forces. J Tissue Viability 1995; 15(4): 26-30.
19. Collins F. Preventing pressure sores in the seated patient. Nurs Stand 1999; 13(42): 50-4.
20. Nursing and Midwifery Council. Code of Professional Conduct. London: Nursing and Midwifery Council, 2002.
21. Norton D, McLaren R, Exton-Smith AN. An investigation of geriatric nursing problems in hospitals. London: National Corporation for the Care of Older People, 1962.
22. Cullum N, Deeks J, Sheldon TA, Song F, Fletcher AW. Beds mattresses and cushions for pressure sore prevention and treatment. Nurs Times 2001; 97(19): 41.
23. Dealey C. Risk assessment of pressure sores: a comparative study of Norton and Waterlow scores. Nurs Stand Spec Suppl 1989; (3): 11-2.
24. Deeks JJ. Pressure sore prevention: using and evaluating risk assessment tools. Br J Nurs 1996; 5(5): 313-4, 316-20.
25. Schoonhoven L, Haalboom JR, Bousema MT, Algra A, Grobbee DE, Grypdonck MH, Buskens E, prePURSE study group. The prevention and pressure ulcer risk score evaluation study. Prospective cohort study of routine use of risk assessment scales for prediction of pressure ulcers. BMJ 2002; 325(7368): 797.
26. Barners J. Preventing pressure sores in wheelchair users. Nurse Prescriber 1996; Nov/Dec: 57-58.
27. Fletcher J. Delivering pressure sore care in the community. Community Nurse 1998; 4(3): 39-40.
28. National Institute for Clinical Excellence. Working together to prevent pressure ulcers. A guide for patients and their carers. London: National Institute for Clinical Excellence, 2001 www.nice.org.uk.
29. Waterlow J. The Waterlow card for the prevention and management of pressure sores; towards a pocket policy. Care Science and Practice 1998; 6: 8-12.
30. Bergstrom N, Braden BJ, Laguzza A, Holman V. The Braden scale for predicting pressure sore risk. Nurs Res 1987; 36(4): 205-10.
31. Wade DT, Collin C. The Barthel ADL Index: a standard measure of physical disability? Int Disabil Stud 1988; 10(2): 64-67.
32. David JA, Chapman R, Chapman EJ. An investigation of the current methods used in nursing for the care of patients with established pressure sore. Harrow: Nursing Practice Research Unit, 1983.