

|
Author(s)
Sue Johnson
|
Contents
|
|
Published:
September
2002
Last updated: September 2002 Revision: 1.0 |
Keywords: venous leg ulcers; compression hosiery; prevention; treatment; guidelines.
Graduated compression hosiery is the recognised gold standard for the treatment of venous ulcers, usually in the form of four-layer bandaging. Unfortunately with some patients the bulkiness of the bandages leads to non-compliance. An alternative to bandaging could be the use of below-knee graduated compression hosiery. This article will review the purpose and function of compression hosiery including details of patient assessment, measurement and compliance issues. It will provide the basic principles that should enable nurses to successfully treat patients with venous ulceration using compression hosiery.
It is estimated that leg ulceration currently affects 580 000 individuals in the UK at any one time and costs approximately Ł300-600 million per annum [1]. The majority of leg ulcers (approximately 70%) are caused by venous disease and recurrence rates are high, with two thirds of patients experiencing one or more recurrences [2]. The central role of compression therapy in the management of venous leg ulcers has been summarised in a systematic review [3]. Graduated compression hosiery is accepted as an integral part of the management of varicose veins and/or leg ulcers [4], both as an active treatment for healing of ulcers [5] and having an essential role in the prevention of venous ulcer recurrence [6].
To ensure adequate venous return from the lower limbs, the superficial veins, deep veins, bicuspid valves and the calf muscle must all work together [7]. The deep veins carry blood back up the leg and consist of two posterior tibial veins, two anterior tibial veins and two peroneal veins which join up to form the popliteal vein which in turn continues into the femoral veins. These veins are situated deep in the muscles of the leg and are protected by a fibrous fascia. The large volume of blood carried by these veins results in a high pressure within the vein walls [8] whereas the superficial veins, consisting of the long saphenous veins, short saphenous veins and numerous superficial collaterals, satellites and confluents of the saphenous veins (Figure 1), carry a smaller volume of blood at a lower pressure. The superficial veins drain into the deep veins by means of the perforating veins. Bicuspid valves, present in both superficial veins and deep veins, ensure that the flow of blood is unidirectional and when these valves are competent they prevent a backflow of blood from the deep veins to the superficial veins.
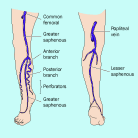
The power to drive the blood back up the leg is provided by the calf muscle, which on walking contracts and relaxes in a regular movement. The contraction of the calf muscle forces the blood upward out of a segment of vein; backflow is prevented by the valve [7]. Relaxation of the calf muscle allows the now empty segment of deep vein to refill with blood from the superficial veins and thus the cycle is repeated.
When valves become incompetent the cycle of unidirectional blood flow is interrupted and backflow of blood occurs (Figure 2). This is most significant when the backflow occurs between the deep and superficial veins, as the increased pressure in the superficial veins will cause further valve incompetence. This is because the valve cusps no longer meet as a result of the stretching of the veins. The overall effect of this increased superficial hydrostatic pressure is the formation of tortuous varicose veins [9].
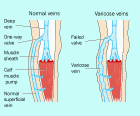
If this increased hydrostatic pressure is not treated it leads to chronic venous insufficiency [9], which in turn results in oedema, lipodermatosclerotic changes, varicose eczema and leg ulceration.
External compression applies controlled pressure to the skin. This then supports the superficial venous system, helping to reduce the increased hydrostatic pressure and redress the balance between the deep and superficial veins (Table 1). This helps in reducing oedema and aiding venous return.
| Increases: |
|
| Decreases: |
|
| Adapted from Ruckley 1992 [10] | |
Unlike compression bandaging with its high working pressure, compression hosiery exerts a resting pressure. The daily build-up of pressure is controlled by the limited ability of the hosiery to stretch, so incompetent venous valves are approximated, venous return is accelerated, the fibrinolytic activity of the venous wall is increased and the risk of thrombosis reduced.
Graduated compression hosiery exerts an external pressure which is greater at the ankle (minimum of 14 mmHg) and reduces at the calf and thigh, thus increasing blood velocity within the deep venous system [11].
How much pressure to apply remains subject to debate, but it is recognised that the amount of pressure required is dependent on the severity of the condition [7], [12]. Severe venous hypertension is associated with oedema, eczema, skin pigmentation, induration and ulceration [13]. It can be seen that the management of these conditions will require a higher level of compression than conditions such as mild varicose veins and oedema (Table 2).
| Class | Pressures | Support | Indications for use |
| I | 14-17 mmHg | Light |
Varicose veins Mild oedema |
| II | 18-24 mmHg | Medium |
Severe varicose veins Mild oedema Prevention of ulcer recurrence |
| III | 25-35 mmHg | Strong |
Severe varicose veins Post-phlebitic limb Prevention of ulcer Recurrence Chronic venous insufficiency |
| Adapted from Scholl 1996 [14] | |||
Haemodynamic studies on compression hosiery show that following removal of the hosiery there is little evidence of reversal of the underlying disease process such as improvement in calf muscle function or restoration of the valves [10]. It is essential that patients are made aware that use of graduated compression forms part of a long-term management plan.
To help identify the most appropriate level of compression, hosiery is divided into three categories. It should be noted that there is a difference in the recommended levels of compression between the European standards and the British standards with the European recommended levels being higher then the UK recommended levels [15]. Hospitals tend to prescribe stockings which meet the European (Hohenstein) method of pressure testing whereas the Drug Tariff [16] supply stockings which meet the Hosiery and Allied Trades Research Association method [17]. The differences between these two specifications are clinically significant, first in the "strength" of the stockings and also in the quality of the materials used to manufacture the stockings. Therefore, it can be seen that a class II stocking supplied to a patient by a GP will apply 18-24 mmHg while the same patient supplied with stockings from a hospital orthotic department will receive 25.2-32.3 mmHg (European standard). With a class III stocking, which is seen to be more beneficial in reducing ulcer recurrence, the patient will receive 25-35 mmHg on a GP prescription and 36-46 mmHg on a hospital prescription [18]. With this discrepancy in strength, and because the GP prescription stockings are easier to apply and more comfortable, patients may decline to wear the hospital prescription stockings as they are more difficult to put on [19]. This fact was recognised in two studies which concluded that it was better to receive a lower compression or lower class stocking than no compression at all [18], [19].
Compression hosiery is classified as class I, II or III depending on the performance of the materials and its indication for use (Table 2). Although class III is the most effective in reducing venous ulcer recurrence [20], better levels of compliance are attained with a class II garment. In patients with manual dexterity problems or the elderly the application of two class I stockings is an alternative to using a class II garment. If two class I stockings are applied one of these may be removed at night.
There are several types of compression hosiery:
Circular knit stockings. These are available in nylon and cotton yarn, and modern stockings substitute elastane for rubber. One disadvantage of these stockings is their lack of stretch, which makes them difficult to put on.
Flat-bed knit stockings. These are available in nylon, cotton and nylon-plated varieties. Nylon stockings have the least ankle pressure, cotton stockings are the most comfortable and nylon-plated stockings are the most durable. Flat-bed knit stockings are more flexible than circular knit stockings, making them easier to get on and off.
Net stockings. These are cut out of net fabric and are seamed, so are the least cosmetically accepted stockings. They are only available as a made-to-measure item.
One-way stretch stockings. These are available only as made-to-measure stockings and are a very heavy circular machine knit stocking.
Few of the fibres used to make modern compression stockings cause allergies, although allergies to rubber used to be a problem.
Compression hosiery is available as thigh-length and below-knee stockings, socks and tights and comes in made-to-measure or standard sizes. A standard size sock is often more acceptable to men than a stocking. Although all stockings and socks are available on Drug Tariff, tights are not available. It should be noted that there is no evidence to suggest that above-knee stockings are more effective than below-knee stockings in correcting underlying pathology [21], [22] whereas ill-fitting thigh-length stockings can encourage pooling of blood lower in the leg [23].
A choice of colour is often available, although flesh coloured is the most often prescribed as women can then wear coloured tights over the top to coordinate with their clothing. The foot can be either open or closed toe, depending on patient preference, and individual requirements can be accommodated in made-to-measure garments but these usually cost extra.
It is important for the clinician to assess the individual patient and each limb for suitability for compression treatment before application. Documentation of the patient's clinical history, physical examination and assessment of the individual's attitude and level of knowledge regarding their diagnosis and compression therapy, can help in the planning of individualised care.
Adopting a systematic approach to assessment will help to identify the most suitable type and class of stocking required.
The physical assessment must include:
Evaluation of the peripheral limb circulation. This is achieved by the use of a Doppler ultrasound to estimate the ankle brachial pressure index (ABPI). High levels of compression are contraindicated when there is significant arterial impairment
Consideration of the patient's age, dexterity and any other disabilities. This will influence the type of hosiery prescribed.
Skin assessment. It is important to check for areas of vulnerability, especially newly healed ulcers where the skin is friable. Vulnerable areas may need protection.
Allergies. Possible allergens should be noted. Elastane, nylon and Lycra are all used in varying amounts in the production of compression hosiery. To reduce potential allergies all fibres are coated with cotton. Where a patient is shown to be allergic to one of the fibres use of a cotton tubular bandage under the stocking could prevent irritation.
Accurate measurement is essential to ensure that hosiery fits properly. A stocking that fits correctly will produce an effective graduation in pressure and will be comfortable to wear without forming tight bands at the knee. Incorrect measurement could result in trauma, discomfort and possible ulceration [20].
Once the style of hosiery has been selected the leg should be measured. To minimise the effects of oedema the leg should be measured either first thing in the morning or as soon as possible after the removal of compression bandages. Measurements should be taken with the patient's feet flat on the floor and both legs should be measured as variation between limbs can occur. Three measurements are required for below-knee stockings:
The ankle at the narrowest point above the ankle bone
The base of the heel to just below the knee
The calf at its widest point.
Five measurements are required for thigh-length stockings:
The above three measurements
The widest part of the thigh
The length from the base of the heel to the gluteal fold.
Once the measurements have been taken the correct size of hosiery can be selected by checking the range into which the measurements fall with the different manufacturer's charts. Charts can usually be obtained free of charge from the manufacturers. These charts detail the ankle, calf and thigh measurements and the corresponding hosiery required. Measurements that fall outside these parameters will mean that made-to-measure hosiery is required. It is generally accepted by clinicians that in the majority of cases below-knee stockings are as effective as thigh-length stockings [10], but individual preference should be taken into consideration. Thigh-length stockings may be indicated where there is swelling above or below the knee or where there is a joint deformity.
Time should be taken to instruct all patients on the correct method of application and how to care for their hosiery (Table 3). All wrinkles should be removed and the patient advised against folding the stockings over at the top. Tight bands at the top of the stocking or over the foot may lead to pressure damage [24]. To avoid damage to the limb and to make application easier the following application technique is recommended:
Insert the hand into the stocking until the seamed heel area is reached
Pinch the heel area between forefinger and thumb and turn the stocking inside out until the heel pocket is visible
Position the stocking over the foot, making sure the heel pocket is correctly positioned over the heel
Pull the remainder of the stocking over the foot and up the leg, positioning the top of the stocking just below the knee/gluteal fold [12].
| Turn hosiery inside out |
| Grasp heal of stocking and pull it through so that it is inside out |
| Position hosiery onto foot and fold over 2-3 inches |
| Take small sections of hosiery and carefully fold up onto leg in sections |
| Having extended stocking to full length, take it back down to midcalf |
| Take sections and with a twisting motion extend up the leg to ensure that the stocking does not slip down |
| Where possible apply a moisturiser the night before |
| Carefully remove hosiery to avoid trauma to newly healed skin |
| Adapted from O'Hare 1997 [25] |
Other tips to aid application (Table 4) are use of rubber gloves, moisturising the leg before application, putting talcum powder on the foot before application and regularly trimming the toe nails.
| Medi Valet | Reduces bending required |
| Chinese slipper | Helps position hosiery onto foot |
| Plastic bag | |
| Nylon stocking | |
| Rubber gloves | Assists grip |
| Talcum powder | |
| Adapted from Edwards and Moffatt 1996 [20] |
A Chinese slipper is often supplied with the stockings, which helps with easing the stocking over the foot. Frames are also available but only direct from the manufacturers or via a hospital orthotic department. Some people find frames helpful and purchasing one for the clinic may be helpful for patients to use before purchasing their own. Compression hosiery should be taken off at night and reapplied first thing in the morning. Regular correct washing can prolong the life of the hosiery - preferably these should be hand washed at 40°C and dried away from direct heat.
Following supply of the hosiery it is advisable to see the patient the following week to ensure there are no problems with applying the stockings and to check that they fit correctly. Patients should be seen at 3-monthly intervals to reassess their peripheral and arterial blood supply and for re-measurement of the limb. New stockings should be supplied every 3-6 months.
Care should be taken when using primary dressings under compression hosiery. If the dressing is not profiled then pressure damage from the edges of the dressing can occur. Also excess padding should not be used under compression hosiery as this will alter the pressure gradient.
Once the ulcer has healed the possibility of surgery for varicose veins should be explored with the patient as it is thought to have an important role in preventing ulcer recurrence [26].
Patient concordance with compression hosiery is problematic [6]. Ensuring concordance is extremely important in the prevention of ulcer recurrence [18]. Awareness of factors that affect concordance will aid assessment and help to plan effective care. The patient's level of knowledge, attitude and motivation, as well as physical constraints which might hinder application and removal of hosiery, are important and should be explored [27]. Some patients may experience difficulty with applying class II stockings in which case it may be advisable to prescribe two class I stockings.
The nurse and patient should work in partnership, with the patient being encouraged to develop an understanding of compression therapy in relation to its function and benefits for them. This will help to develop a positive attitude, fuel motivation and aid concordance. Provision of written leaflets will back up verbal discussions and instructions and continue the education process. This approach is designed to involve the patient in their care and create a sense of responsibility and ownership.
Patient education should also include issues such as exercise, diet, weight, limb elevation and skin care. Exercise should include both active and passive exercises, such as walking and ankle exercises. These exercises all activate the calf muscle pump and complement the effects of compression hosiery.
Although it is recognised that the 'gold standard' for the treatment of leg ulceration is graduated compression bandaging, difficulties will still be experienced with some patients who find the bandages too bulky. In this instance an alternative method of applying graduated compression could be the prescribing of below-knee graduated compression hosiery with an appropriate primary dressing. Recurrence rates for leg ulcers are high, especially where there is non-compliance with compression [6]. The ultimate goal should be to reduce the risk of ulceration in the first place. Appropriate assessment of the pathophysiology of the ulceration, supported by education of patients, carers and healthcare professionals, will enable healthcare professionals to improve patients' quality of life and provide cost-effective care in the treatment of venous insufficiency and leg ulceration.
This article has reviewed the purpose and function of compression hosiery including details of patient assessment, measurement and compliance issues. By applying these principles nurses should have sufficient knowledge to successfully treat their patients with compression hosiery.
1. Department of Health. Gravitational (varicose) ulcers. The problem, what we need to know and what we need to do. HMSO, 1989.
2. Callam M. Prevalence of chronic leg ulceration and severe chronic venous disease in western countries. Phlebology 1992; 1((Suppl)): 6-12.
3. NHS Centre for Research and Dissemination. Compression therapy for venous leg ulcers. Effective Health Care Bulletin 1997; 3: 4.
4. Jeffrey PC, Nicolaides AN. Graduated compression stockings in the prevention of post-operative deep vein thrombosis. Br J Surg 1990; 77: 380-82.
5. Mayberry JC, Moneta GL, Taylor LM, Porter JM. Fifteen-year results of ambulatory compression therapy for chronic venous ulcers. Surgery 1991; 109(5): 575-81.
6. Moffatt CJ, Dorman MC. Recurrence of leg ulcers within a community ulcer service. J Wound Care 1995; 4(2): 57-61.
7. Dale JJ. The anatomy and physiology of the circulation of the legs.. In: Cullum N, Roe B, editors. Leg ulcers: nursing management - a research based guide. Harrow: Scutari, 1995.
8. Hollinworth H. Venous leg ulcers part 1: aetiology. Professional Nurse 1998; 13(8): 553-58.
9. Browse NL, Burnand KG. The cause of venous ulceration. Lancet 1982; 2(8292): 243-5.
10. Ruckley CV. Treatment of venous ulceration: compression therapy. Phlebology 1992; 1: 22-26.
11. Lawrence D, Kakkar VV. Graduated, static, external compression of the lower limb: a physiological assessment. Br J Surg 1980; 67(2): 119-21.
12. Keachie JJ. Prevention of re-ulceration. In: Cullum N, Roe B, editors. Leg ulcers: nursing management - a research based guide. Harrow: Scutari, 1995.
13. Moffatt C, O'Hare L. Graduated compression hosiery for venous ulceration. J Wound Care 1995; 4(10): 459-62.
14. The complete Scholl guide to health care for legs. Luton: Scholl, 1996.
15. Stemmer R, Marescaux J, Furderer C. [Compression therapy of the lower extremities particularly with compression stockings]. Hautarzt 1980; 31(7): 355-65.
16. Dept of Health National Assembly of England and Wales. Drug Tariff. Compression Hosiery. London: The Stationary Office, 2001.
17. (Anonymous). Compression hosiery. The Pharmacy Magazine 2001.
18. Harper D, Nelson E, Gibson B, Prescott R, Ruckley C. A prospective randomised trial of Class 2 and Class 3 elastic compression in the prevention of venous ulceration. Phlebology 1995; 1: 872-73.
19. Travers JP, Dalziel KL, Makin GS. Assessment of a new one layer adhesive bandaging method in maintaining prolonged limb compression and effects on venous ulcer healing. Phlebology 1992; 7: 59-63.
20. Edwards L, Moffatt C. Tissue viability. The use of compression hosiery in the care of leg ulcers. Nurs Stand 1996; 10(31): 53-6.
21. Thomas S. Graduated compression and the prevention of deep vein thrombosis (Part 2). J Wound Care 1999; 8(2): 93-5.
22. Williams AM, Davies PR, Sweetnam DI, Harper G, Pusey R, Lightowler CD. Knee-length versus thigh-length graduated compression stockings in the prevention of deep vein thrombosis. Br J Surg 1996; 83(11): 1553.
23. Sparrow RA, Hardy JG, Fentem PH. Effect of 'antiembolism' compression hosiery on leg blood volume. Br J Surg 1995; 82(1): 53-9.
24. Jones JE, Nelson EA. Compression hosiery in the management of venous leg ulcers. J Wound Care 1998; 7(6): 293-6.
25. O'Hare L. Scholl compression hosiery in the management of venous disorders. Br J Nurs 1997; 6(7): 391-4.
26. Sethia KK, Darke SG. Long saphenous incompetence as a cause of leg ulceration. Br J Surg 1994; 71: 754-55.
27. Dale JJ, Gibson B. Systematic care brings results. Prof Nurse 1993; 8(5): suppl 3-13.