

|
Author(s)
Glen Cousquer
|
Contents
|
|
Published:
Oct 2002
Last updated: Oct 2002 Revision: 1.0 |
Keywords: badgers; terrritorial fight wouunds; wound debridement; wound healing; hydrocolloid dressings.
The social behaviour of the badger is highly complex.
Badgers are commonly presented to rehabilitation centres with territorial fight wounds.
Careful triage and patient selection is essential.
A wound management programme using hydrocolloid dressings is proposed.
The Eurasian badger (Meles meles) is common throughout much of the British Isles with the greatest population density occurring in the South West [1]. Consequently, injured badgers are frequently presented to wildlife hospitals for care and rehabilitation. The two most common 'reasons for admission' for adult badgers presenting to the RSPCA's West Hatch Wildlife Hospital in Somerset are road traffic accidents and territorial fight wounds. This paper reviews the techniques currently used to manage fight wounds and explores some of the issues arising from such interventions.
In the British Isles, badgers live together in social groups in well-defined territories. Defended areas tend to be delineated by territorial latrines and perimeter paths during the first four to five months of the year. During this period aggression between badgers is not unusual and fighting can be particularly severe in high-density areas. Fighting within a social group is, by contrast, unusual although a sow with small cubs will defend a monopolised zone within a sett.
The occurrence of bite wounds in boars appears to peak distinctly in February to March with a less well-defined increase around September [2]. The pattern in sows is different, with a lower overall incidence and less clearly defined peaks occurring in April and November-December. The incidence of fight wounds seen at the West Hatch Wildlife Hospital shown in Figure 1 would tend to support this.
Data from the 2001 season is not included as the Foot and Mouth restrictions drastically affected hospital admissions during the spring. In the 1999 and 2000 seasons, most of the fight wounds were seen in the spring (February - May): 27 (79.4%) in males and 27 (81.8%) in females. No fight wounds were seen in either sex during November to January. It is possible that this spring peak is linked with the main peak of mating behaviour. This occurs between January and May, with older females probably accounting for the main peak in February, and yearlings of 12-14 months for the second peak in April-May.
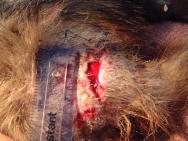
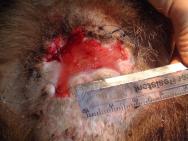
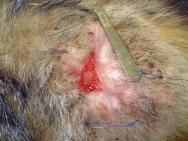
A wide range of fight wounds are seen at the West Hatch Wildlife Hospital, from incidental puncture wounds to large suppurative wounds. Two distinct areas are affected: the rump area is most commonly affected, but there may also be wounds to the neck, throat and shoulder area. Bite wounds often penetrate deep into the dermis, introducing bacteria into the subcutaneous tissues and setting up foci of infection. In some badgers these foci of infection burst out and coalesce, resulting in large open wounds that may subsequently become flyblown (Figure 2). Many badgers cope well with their wounds and it is not uncommon for badgers to be seen at the hospital with incidental wounds, requiring little or no treatment (Figure 3).
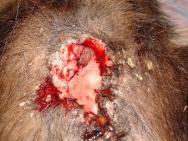
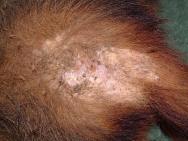
In those badgers with extensive or severely infected wounds the decision to treat, or to euthanase, must take into account a number of important factors. These include:
age
body condition
health status and other injuries
size and condition of the wounds
prospects for return to the wild.
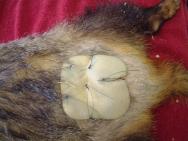
An approximate assessment of age can be made upon oral examination. Severe attrition of the incisor, premolar and molar tables is commonly seen in geriatric badgers (Figure 4). These animals are frequently emaciated (<6kg body weight) and should be euthanased on welfare grounds.
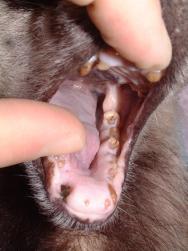
Consideration must also be given to the health status of the badger. A thin individual with large numbers of ectoparasites is likely to be immuno-suppressed and malnourished, and may be suffering from intercurrent disease. Other injuries may also be present and a thorough clinical examination should be performed on all patients. It should be remembered that the badger is the main wildlife reservoir of Mycobacterium bovis. Bacilli may be excreted in the sputum as well as in the urine and faeces, and from suppurative wounds.
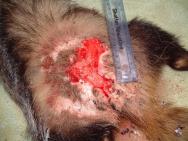
Severely infected wounds, and wounds where there is a large skin deficit, are unlikely to heal quickly (Figure 5).
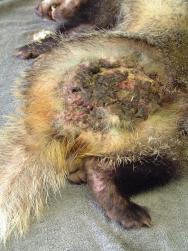
The West Hatch Wildlife Hospital aims to return casualty badgers back to the wild within 4-6 weeks. Badgers are returned to their home area on release, following a site visit and investigation. A map reference must be recorded for the site at which the badger was found and, where possible, an idea of the badger's social status should be established as this may affect its chances of reintegration into a social group. An ousted old boar is, for example, less likely to re-establish itself.
In certain cases, where the injuries will not heal in the space of a month, or where a badger has been driven away from his territory into an urban area, the decision may have to be taken to euthanase the animal. It should be remembered that it is an offence to abandon an animal in a manner that is likely to cause it unnecessary suffering (Abandonment of Animals Act 1960), and one must be reasonably confident that a rehabilitated badger will be able to compete on equal terms with its peers in the wild. All badgers released from the West Hatch Wildlife Hospital are identichipped and tattooed (under licence). It is hoped that this will provide some post-release data to help evaluate the success of the treatment and rehabilitation of these badgers.
Following careful triage and case selection, the badger should be relatively healthy, with good release prospects, and whose wound(s) require careful management to ensure the shortest possible stay in captivity. A method of treatment has been developed at the West Hatch Wildlife Hospital to promote rapid wound healing.
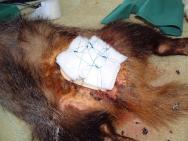
On admission the wound is subject to aggressive debridement under general anaesthetic. Any necrotic tissue is excised and the wound liberally flushed with Dermisol (a propylene glycol, malic acid, benzoic acid and salicylic acid solution) to promote sloughing of any remaining devitalised tissue. Nylon stay sutures are then placed in healthy tissue around the wound (Figure 6). These will be left in-situ for the duration of the treatment. A hydrocolloid dressing (Granuflex) is then applied over the wound. Use of an alcohol-based skin disinfectant (Vetasept) to clean the surrounding skin provides a clean, fast-drying, surface for the dressing to adhere to. Swabs can be placed over the dressing to provide padding. A piece of nylon is then laced, in a zig-zag fashion, through the stay sutures to further secure the dressing (Figure 7 and Figure 9). Dressings can be stapled in place, although this technique is more costly, especially if multiple dressing changes are required.
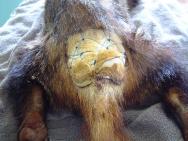
The dressings are surprisingly well tolerated and I have only come across one badger who insisted on removing and eating the dressings. This particular problem was resolved by overlaying a few strips of elastoplast over the hydrocolloid dressing and stapling these down - a 'no-nonsense solution' that proved very effective.
Initially dressings may need to be changed every 3 to 4 days. Once all infection has been eliminated from the wound, the volume of wound discharge reduces and dressings can be left in place for up to 7 days. Each dressing change is performed under general anaesthetic, a procedure which causes minimal stress to the patient, with induction occurring within 2 to 3 minutes of entering the badger's pen.
Rump wounds pass through three distinct phases. During the first phase the wound moves from an infected to a healthy state. During this time the badger receives oral clavulanate-amoxycillin (Synulox) at a dose rate of 250 mg per day (equivalent to 25 mg/kg for a typical 10 kg badger). Cost precludes routine swabbing of wounds for culture and sensitivity testing. Swabbing would only be considered where wound infection was proving resistant to treatment; consideration would then also be given to testing for Mycobacterium bovis. Chemical debridement, using a propylene glycol, malic acid, benzoic acid, salicylic acid solution (Dermisol), at each dressing change, continues until all necrotic tissue has been eliminated from the wound. During the second phase a bed of granulation tissue is established in the healthy wound. At the time of each dressing change the wounds are lavaged with 0.9% sterile saline to remove any wound exudate. During the third phase the wound starts to epithelialise and contract. Wound contraction is responsible for the greatest part of wound closure. This is very important as the thin layer of new epithelial tissue would provide little protection.
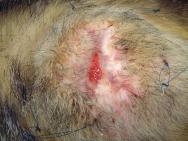
The progress of an especially large wound is illustrated in Figures 8-13. This particular badger presented with a large wound; the wound was fairly old and was surrounded by nodules of scar tissue. A bed of granulation tissue was well established and the wound was essentially healthy (Figure 8). A dressing was applied to the wound on day 2 after presentation (Figure 9). Dressing changes took place on day 5 and then on day 9. By this time there was evidence of good epithelialisation around the edges of the wound (Figure 10). Thereafter dressing changes occurred at weekly intervals. Figure 11 illustrates a week-old dressing that is firmly secured over the wound. By day 30 the wound had contracted dramatically (Figure 12) and now measured 3 cm at its widest point. By day 37 further contraction had occurred and the wound was deemed healthy enough to be left without any dressing to protect it (Figure 13). The stay sutures were removed and the wound left to scab over. A coconut oil based fly repellent (Xenex) was applied to the surrounding skin to ward off any flies. The badger was released after a stay of less than 40 days in the hospital.
The use of hydrocolloid dressings has a number of very valuable benefits:
The wound environment is stabilised
Further contamination of the wound is prevented
The conditions for wound healing are optimised
The badger's welfare is significantly improved.
Previous treatments for badger rump wounds used in the hospital consisted of the daily application of hydrogels (Intrasite). Badgers were bedded on blankets, instead of hay and sawdust to keep the wounds clean. By using a hydrocolloid wound dressing, the handling and disturbance of each badger is reduced. In addition, the superior protection provided by these dressings enables them to be bedded on hay and sawdust; these are more natural materials and allow the badger to exhibit normal nesting behaviour. Stress levels are considerably reduced in this manner - something which can only benefit wound healing. The creation of a moist and stable environment over the wound protects the underlying tissues and promotes rapid granulation and epithelialisation. The surgical repair of a rump wound using a fasciocutaneous transposition flap has been attempted [3], but was unsuccessful. By contrast the method of treatment developed at the West Hatch Wildlife Hospital to promote rapid wound healing is cheap, reliable and easy to perform.
1. Cresswell P, Harris S, Jaffries DJ. The history, distribution, status and habitat requirements of the badger in Britain. Peterborough: Nature Conservancy Council, 1990.
2. Cresswell WJ, Harris S, Cheeseman CL. To breed or not to breed: an analysis of the social and density-dependent constraints on the fecundity of female badgers, Meles meles. Phil Trans R Soc Lond 1992; 338: 393-407.
3. Keeble E. Surgical treatment of a territorial fight wound in a badger (Meles meles) - a novel technique. In: Proceedings of the BVZS Autumn Meeting, Nov 20-21, 1999; British Veterinary Zoological Society, London, 53-54.
Neal E, Cheeseman C. Badgers. London: T & AD Poysner Natural History, 1996.