

| Dr S Thomas, Director Surgical Materials Testing Laboratory Bridgend District and NHS Trust, Bridgend H.N. Rowe, J Keats, Dr R.J.H. Morgan, |
Contents
Summary Submitted: 25 August 1997 |
This article describes a technique for the treatment of extravasation injuries in neonates, in which the affected area is covered with a sterile amorphous hydrogel enclosed in an impermeable plastic bag or sleeve. The authors discuss potential advantages of this technique over alternative methods for treating such injuries, by reference to selected case histories.
Extravasation injuries are a potentially serious consequence of all intravenous therapy, but they are generally associated with the administration of antineoplastic agents or osmotically active solutions containing 10 per cent glucose, calcium chloride or calcium gluconate. [1] [2] [3]
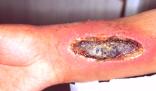 Figure 1 - Extravasation
injury on an adult's wrist
Figure 1 - Extravasation
injury on an adult's wrist
Patients of all ages may be affected, but a retrospective review of 31 cases over a nine-year period showed that they occurred primarily in children and older people [2], with 57 per cent of all injuries occurring on the hand or dorsum of the foot. Most of the resulting lesions produced severe scarring and loss of function, many required surgical intervention and in a number of cases amputation was necessary.
Neonates and premature babies are particularly at risk of developing extravasion because of the small size of their vessels and the immature structure of their skin. The structure and function of skin in the newborn has been described by Young. [4]
A two-year retrospective study of complications related to neonatal infusion sites revealed that skin loss secondary to extravasation had occurred in 33 babies, equivalent to 2.4 percent of all admissions. [5]
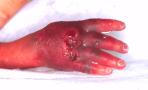 Figure 2 - Extravasation
injury on the hand of a newborn infant
Figure 2 - Extravasation
injury on the hand of a newborn infant
Of the 33 cases, nine developed severe scarring requiring plastic surgery, or contractures severe enough to interfere with function. In all nine infants, the injury occurred on the lower leg of dorsum of the foot.
 Figure 3 - Extensive
extravasation injury on lower leg
Figure 3 - Extensive
extravasation injury on lower leg
Published methods of preventing and treating such injuries include the elevation of the affected limb, application of hot and cold packs, the local administration of corticosteroids or hyaluronidase and the use of specific antidotes where available. [6] Liposuction and and saline flushes (with or without a pretreatment with hyaluronidase) have also been recommended. [7]
A massage technique which is claimed to reduce scarring and the need for grafting has been described by Davidson et al., [8] It is claimed that this technique frees the epithelial margin from the central coagulum present in the wound, overcoming the contracting effects of myofibroblasts present in the granulation tissue. In this technique the necrotic tissue and, presumably the wound itself are allowed to dry out and demarcate, an approach which is not in accord with the current philosophy of moist wound healing.
The current treatment was developed specifically for treating extravasation injuries in the hands or feet of small infants but it can easily be adapted for treating similar injuries in patients of all ages.
The technique involves the use of a sterile amorphous hydrogel applied to the affected area in a sterile polythene bag forming a "glove" or "boot".
 Figure 4 - Extravasation injury
in glove containing hydrogel
Figure 4 - Extravasation injury
in glove containing hydrogel
The latter can be conveniently produced from a sterile disposable examination glove using a domestic heat sealer of the type used for packaging food prior to storage in a deep freeze.
If such equipment is not available, sterile urine collection bags may be used. These are widely available in special care baby units, although they tend to be made from less conformable plastic than that used in examination gloves.
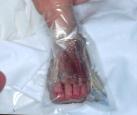 Figure 5 - Extravasation injury
dressed with a boot made from a urine drainage bag
Figure 5 - Extravasation injury
dressed with a boot made from a urine drainage bag
The treatment may be started as soon as extravasation is detected or suspected, but should not preclude the use of other more immediate or specific measures such as removal of the extravasated drug by needle aspiration if there are more obvious signs of fluid swelling. If tissue damage is apparent, treatment should be started immediately.
The technique is simple to perform. Gel is applied liberally to the injury and the affected limb is placed inside the plastic bag. If required, additional gel may be delivered into the bag with a syringe and a quill using a sufficient to ensure that the wound remains covered at all times and that the bag does not come into contact with the wound surface.
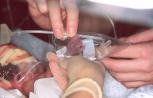 Figure 6 - Application of
hydrogel using a syringe and quill
Figure 6 - Application of
hydrogel using a syringe and quill
The neck of the bag is closed using surgical tape ensuring that the tape does not come into contact with the baby's skin. If necessary a splint may be applied to the affected limb to support the weight of the gel. As both the gel and the bag are transparent, the wound may be examined without disturbing the dressing, which can usually be left in place for two to three days. If the wound shows any clinical evidence of infection the dressing should be replaced daily and appropriate antibiotic therapy initiated.
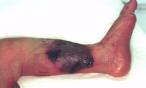 Figure 7 - Extravasation injury
on leg prior to treatment with hydrogel
Figure 7 - Extravasation injury
on leg prior to treatment with hydrogel
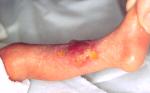 Figure 8 - Injury during
treatment with gel
Figure 8 - Injury during
treatment with gel
Dressings changes are accomplished by gently sliding the bag off the limb and irrigating the wound with sterile isotonic saline. During this treatment it should not be necessary to touch the surface of the wound which does not need to be dried before the dressing is replaced.
To prevent unnecessary cooling of the surface of the wound, both the gel and the normal saline should be warmed to body temperature prior to use, as it has been shown that a temperature below 28 ° C will reduce mitotic and phagocytic activity and thus delay healing. [9]
During healing, a pale-yellow semi-solid fibrinous layer may develop on the wound surface. This layer does not appear to effect the healing process and need not be removed.
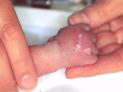 Figure 9 - Injury part
way through treatment showing fibrinous covering to wound
Figure 9 - Injury part
way through treatment showing fibrinous covering to wound
In laboratory studies it has been shown that hydrogels not only prevent the growth and proliferation of innoculums of bacteria but that they also exert a mild bactericidal effect due, it is presumed, to the propylene glycol that most contain. [10]
Figure 10 shows an injury resulting from extravasation which occurred during a blood transfusion. An area of full thickness skin loss can be seen, surrounded by massive bruising. The wound was dressed as described and the dressing changed every three days. The healed wound, photographed four weeks later, is shown in Figure 13.
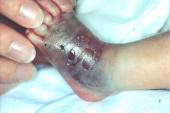 Figure 10 -
Extravasation prior to treatment
Figure 10 -
Extravasation prior to treatment
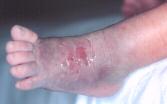 Figure 11 - Injury
during treatment
Figure 11 - Injury
during treatment
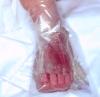 Figure 12 - Boot in
place
Figure 12 - Boot in
place
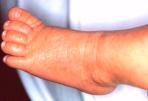 Figure 13 - Healed
wound
Figure 13 - Healed
wound
The gel that was used during the original study was Scherisorb - Smith & Nephew Medical Ltd. This contained 2% of a starch co-polymer, 80% water and 20% propylene glycol as a humectant and preservative. This particular formulation is no longer available, but it is likely that many of the new amorphous hydrogels such as Intrasite - Smith and Nephew Medical, Granugel - Convatec Ltd and Sterigel - Seton Healthcare that have since appeared on the market will be equally as effective.
Amorphous hydrogels are used extensively for the treatment of sloughy or necrotic lesions where they are believed to facilitate autodebridement of the wound by rehydrating slough and enabling autolysis to take place at an enhanced rate.
In the current application, the gel also prevents dehydration of damaged tissue and limits further devitalisation of exposed dermis. These properties are particularly important in view of the high room and incubator temperatures which are required in a special care baby unit.
The use of the gel also appears to decrease or prevent excessive wound contraction and scarring, achieving the same effect as the massage technique described previously. [6]
It is interesting to speculate whether in an uncovered wound the production and subsequent contraction of myofibroblasts is initiated or enhanced by the partial dehydration of the granulation bed as a result of the loss of water vapour from the exposed tissue.
When used in the manner described, the gel would prevent this water loss, inhibit contraction and maintain the viability of the wound and surrounding tissue.
Our experience with this technique suggests that it offers the following benefits:
This article contains information that was originally published in a paper in the Pharmaceutical Journal. This information is reproduced here by kind permission of the editor.