Recent advances in the use of lasers in dermatology.
Abstract
Lasers have been used in dermatology for more than 20 years. The first
lasers used were the Ruby and Argon lasers, and a great deal of experience
has been obtained particularly with the latter. The Argon laser has been
used predominantly in the treatment of cutaneous vascular lesions and the
CO2 laser both as a cutting and ablating tool.
There have been significant advances in the development and use of dermatological
lasers. Much of this development stems from the close co-operation of scientists
and clinicians and laser manufacturers. Today's lasers are more specifically
designed for a narrow range of applications and have significant advantages
over older lasers. This article will review the use of the flashlamp-pulsed
tunable dye laser in the treatment of port wine stains, and developments
in the treatment of tattoos and cutaneous pigmented disorders, and skin
resurfacing.
Flashlamp-pumped pulsed tunable dye laser treatment.
For over 20 years, the Argon laser has been the most widely used laser
for the treatment of cutaneous vascular lesions
[1].
The Argon laser emits blue and green light at 488 and 514 nm. These wavelengths
of light are preferentially absorbed by oxyhaemoglobin and melanin in the
skin[2]. The light energy absorbed by
erythrocytes within blood vessels is converted to heat, leading to red
cell destruction and thrombosis of small blood vessels.
Port wine stains
Port wine stains [PWS] are benign vascular birthmarks which consist of
ectatic capillaries within the superficial dermis[3].
PWS persist throughout life and cause significant psychological disability[4].
Light from the Argon laser produces selective damage to the ectatic blood
vessels within a PWS and results in significant lightening of the skin[3,5].
Most large series of patients treated with this laser have reported good
and excellent results in 60 - 80% of patients[6].
Best results have been in dark purple PWS in adults, worst results in children
with pink, easily compressible PWS. Unfortunately the incidence of scarring
after Argon laser treatment is significant, with textural changes occurring
in up to 22% of patients. [Fig.1]
Fig. 1
Scarring after Argon laser treatment of a port wine stain

(click on image for full size illustration)
Histological assessments of Argon laser treated PWS have demonstrated
that although the light is selectively absorbed by haemoglobin, the damage
induced is relatively non-specific[7,8].
These changes are in part due to non-selective absorption of the Argon
laser light by other chromophores such as melanin, and diffusion of thermal
energy away from targeted blood vessels to adjacent structures due to the
long [ms] laser pulses employed[9]. Analysis
of the optical properties of PWS skin has suggested different parameters
to those of the Argon laser for successful treatment of these naevi[10,11].
Light with a wavelength of 577 nm coincides with the beta absorption peak
of oxyhaemoglobin and was the original wavelength used in flashlamp-pumped
pulsed dye lasers[12]. Preliminary studies
revealed high response rates with minimal complications. Penetration depth
can be increased from 0.5 to 1.2 mm in PWS skin, whilst maintaining the
same degree of vascular selectivity, by increasing the wavelength of light
from 577 to 585 nm[13] . It is possible to
confine thermal injury to targeted blood vessels, without heat diffusion
to surrounding tissues, by using microsecond pulses [Table 1].
Table 1: Treatment parameters of flashlamp-pumped pulsed dye laser.
| Wavelength |
585nm |
| Pulse Duration |
450µs |
| Spot size |
5-10 mm |
| Energy fluence |
5-9 J/cm2 |
Histological studies have confirmed the selective vascular injury induced
by this laser with minimal damage to the overlying epidermis. Videomicroscopic
analysis of treated skin has confirmed that there is no thermal damage
to the epidermis[14].
The significant advantage of this laser is its safety and efficacy in
children with PWS and low incidence of scarring[15-17].
Treatment in older children and adults is well tolerated, local anaesthesia
(EMLA cream) often being adequate[18].
Younger children may require repeated general anaesthetics. The laser produces
marked bruising which can persist for up to 2 weeks, although crusting
and weeping is much less common than with other lasers.
Treatments to the whole port wine stain are generally repeated every
6 - 12 weeks and a course of treatment is prolonged, 10 or more treatments
often being necessary. Not all patients will clear; the site of the PWS
will influence outcome[19]. Recent work
analysing the pattern of vascular ectasia within a PWS using a videomicroscope
has identified patterns of ectasia associated with good and poor outcomes
from pulsed dye laser therapy[20]. Patients
with ectasia of the superficial capillary loops had a better outcome than
those with ectasia of the horizontal vascular plexus. Further work may
enable a more accurate prognosis for outcome of treatment. Best results
have been on facial PWS and worst results on the lower limbs[21].
[Fig 2a & b].
Fig. 2a & b. Facial port wine stain before and after pulsed dye
laser
therapy
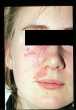 click on image for full size illustration
click on image for full size illustration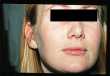
Hyperpigmentation may be a problem, particularly following treatment
of PWS on the leg. Scarring is rare without additional trauma in the post-treatment
period[22]. This laser is also reported
to be of value in hastening the resolution of strawberry haemangiomas[23,24],
particularly if the strawberry haemangioma is causing complications such
as ulceration or bleeding, but controlled studies are lacking. Treatment
should be performed early for any benefit[25].
However the flashlamp-pumped dye laser can also produce satisfactory changes
in residual haemangiomas with a prominent telangiectatic component.
Tattoos
Tattoos often applied in teenage years may become a source of regret and
a social burden in later life[26]. A number
of methods of removal of tattoos have been employed including dermabrasion,
salabrasion, cryotherapy and excision. Surgical excision of large tattoos
requires skin grafting. The other methods suffer from the disadvantages
of incomplete pigment removal, necessity of repeated procedures, pain and
frequent scarring. Carbon dioxide laser therapy[27]
removes tattoo pigment after vaporization of the epidermis and superficial
dermis. Although effective, this laser has a high incidence of scarring
and pigmentary disturbances. "Q-switching" whereby high energy levels [5
- 10 J/cm2] delivered in ultrashort pulse widths [10 - 80 ns]
of Ruby, Nd:YAG and Alexandrite lasers has offered significant advances
in the treatment of tattoos, particularly blue-black amateur tattoos[28-30]
[Fig 3a & b].
Fig. 3a & b. Amateur tattoo on shoulder treated once with the
Q-Switched Nd:YAG laser.
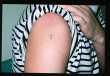 click on image for full size illustration
click on image for full size illustration
The light emitted by these lasers interacts with dermal pigment within
tattoos and produce selective removal of the pigment, partly by photomechanical
disruption of the pigment granules[31].
Ruby lasers emit light at 694 nm and Nd:YAG lasers at 1064 nm. Both lasers
produce best results in blue-black tattoo pigments. The Ruby laser can
also be used to treat green tattoos[32].
Frequency doubling of Nd:YAG laser light halves the wavelength to 532 nm
producing green light. This green light can produce fading of red tattoo
pigments[33]. The Alexandrite laser with
a wavelength of 755 nm produces slower results than the other two Q-Switched
lasers but may be of value in the treatment of other coloured tattoo pigments[34].
These lasers produce much less epidermal reaction than other methods of
tattoo removal particularly if large laser beam diameters are used. There
is a consequent reduction in the incidence of scarring following treatment.
Hypopigmentation following Ruby laser treatment may be a problem.
Cutaneous pigmented lesions
As melanin absorbs across a wide part of the electromagnetic spectrum,
older lasers with long pulse durations have been employed with some success
in the treatment of pigmented cutaneous lesions[35].
Non-specific thermal damage following heat diffusion to other cutaneous
structures resulted in scarring in some cases. Q-Switched lasers have been
used to treat cutaneous pigmented lesions with some success[36-39].
Both epidermal and dermal pigmented lesions may respond, such as cafe au
lait macules, lentigines and naevus of Ota [Fig 4a & b].
Fig. 4a & b. Benign lentigo treated twice with the Nd:YAG laser.
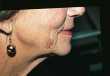 Click on image for full size illustration
Click on image for full size illustration

Repeated treatments may be necessary and the lesion may recur. There
is insufficent data concerning laser treatment of benign melanocytic naevi
to recommend this form of treatment[40,41].
It is not possible currently to determine which laser is more successful
in this field as few authors have presented data on large series of patients.
However, preliminary work from Japan on 200 naevus of Ota patients treated
with the Nd:YAG laser has revealed impressive results in some patients[39].
Q-Switched lasers have a low incidence of adverse reactions in this group
of conditions. The Alexandrite laser theoretically may also be of value
in the treatment of pigmented lesions although there is little published
clinical work to support this as yet. A flashlamp-pumped pulsed dye laser
emitting light at 510 nm has also been used in the treatment of pigmented
lesions[42,43]. Again short pulse
durations [300 ns] and high peak powers [approximately 4 MW] are utilised
to produce selective photothermolysis of pigment-containing cells.
Carbon Dioxide Laser
The carbon dioxide laser emits infrared light at 10,600 nm. This wavelength
is absorbed by tissue water and the laser produces non-selective thermal
damage of tissue. This laser is used widely in gynaecological surgery and
has been used to treat a number of dermatological disorders. The laser
can be used in focused mode with a small spot size and high energy densities
to cut tissue haemostatically as small blood vessels are sealed thermally.
In the defocused mode, with a spot size of 2 mm, the laser can be used
for superficial vapourisation under local anaesthesia[44].
A variety of skin diseases have been treated with this laser[45-48].
This laser has a relatively high incidence of scarring and other hazards
include human papilloma virus DNA present in the smoke plume generated
when treating warts[49] [Fig 5].
Fig. 5 Smoke plume during CO2 treatment of verruccae
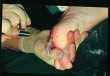 click on image for full size illustration
click on image for full size illustration
A resurgence of interest has developed in the CO2 laser
by the use of ultrapulses of the light. Pulse durations of 250 µs
are delivered which allows thermal destruction of the epidermis and superficial
dermis without thermal diffusion to deeper tissue. The laser can be linked
to an optomechanical scanner for improved results. The laser has an increasing
role in the treatment of photodamaged skin and rhytides[50].
Both ablation of tissue and dermal shrinkage are considered important mechanisms
in the improvement of photodamaged skin[51].
The latter has been measured objectively[52].
Careful pre and post operative preparations are necessary to reduce the
risk of adverse reactions which include scarring, post inflammatory pigmentary
disturbances, persisting erythema, bacterial and viral infections.
Conclusions
The newer generation of lasers with short pulse durations and high peak
powers are capable of more selective destruction of target chromophores.
More appropriate wavelength selection for different cutaneous disorders
has resulted in a modest improvement in results of treatment and a substantial
reduction in adverse reactions such as scarring and pigmentary disturbances.
The flashlamp-pulsed dye laser has enabled the safe treatment of young
children with PWS, and Q-Switched lasers have been effective in the treatment
of a number of cutaneous pigmented disorders, in particular blue-black
tattoos. Further research will clarify which, if any, is the "best" laser
in this second group; significant advances in technology and clinical results
offer an optimistic future in this field.
Acknowledgement
The author acknowledges the support of the Disfigurement Guidance Centre,
Cupar, Fife, Scotland.
References
-
Spicer M S, Goldberg D J. Lasers in dermatology.
J Am Acad Dermatol 1996; 34: 1 - 25.
-
Anderson, R. R., Parrish, J. A. The optics of human
skin. J Invest Dermatol 1981; 77: 13 - 19.
-
Noe, J. M., Barsky, S. H., Geer, D. E., Rosen, S. Port
wine stains and the response to argon laser therapy: successful treatment
and the predictive role of colour, age and biopsy. Plast Reconstr Surg
1980; 65: 130 - 36.
-
Lanigan, S. W., Cotterill, J. A. Psychological disabilities
amongst patients with port wine stains. Br J Dermatol 1989; 121:
209 - 215.
-
Carruth, J. A. S. The argon laser in the treatment
of vascular naevi. Br J Dermatol 1982; 107: 365 - 368.
-
Apfelberg, D. B., Flores, J. T., Maser, M. R.,
Lash, H. Analysis of complications of argon laser treatment of port wine
haemangiomas with reference to striped technique. Lasers Surg Med
1983; 2: 357 - 371.
-
Finley, J. L., Arndt, K. A., Noe, J., Rosen, S. Argon
laser - port wine stain interaction. Immediate effects. Arch Dermatol
1984; 120: 613 - 619.
-
Greenwald, J., Rosen, S., Anderson, R. R. et al.
Comparative histological studies of the tunable dye [at 577 nm] laser and
argon laser. The specific vascular effects of the dye laser. J Invest
Dermatol 1981; 77: 305 - 310.
-
Tan, O. T., Carney, M., Margolis, R., et al. Histologic
responses of port-wine stains treated by argon, carbon dioxide and tunable
dye lasers. Arch Dermatol 1986; 122: 1016 - 1022.
-
Van Gemert, M. J. C., Welch, A. J. Treatment of port-wine
stains: analysis. Med Instrum 1987; 21: 213 - 217.
-
Anderson, R. R., Parrish, J. A. Microvasculature
can be selectively damaged using dye lasers: a basic theory and experimental
evidence in human skin. Lasers Surg Med 1981; 1: 263 - 76.
-
Morelli, J. G., Tan, O. T., Garden, J et al. Tunable
dye laser [577 nm] treatment of port wine stains. Lasers Surg Med
1986; 6: 94 - 99.
-
Tan, O. T., Murray, S., Kurban, A. K. Action spectrum
of vascular specific injury using pulsed irradiation. J Invest Dermatol
1989; 92: 868 - 71.
-
Motley, R. J., Katugampola, G, Lanigan, S. W. Microvascular
abnormalities in port wine stains and response to 585 nm pulsed dye laser
treatment. Br J Dermatol 1996; 135: Suppl 47: 13 - 14.
-
Garden, J. M., Polla, L. L., Tan, O. T. The treatment
of port-wine stains by the pulsed dye laser. Arch Dermatol 1988;
124: 889 - 96.
-
Polla, L. L., Tan, O. T., Garden, J. M., Parrish,
J. A. Tunable pulsed dye laser for the treatment of benign cutaneous vascular
ectasia. Dermatologica 1987; 174: 11 - 17.
-
Tan, O. T., Sherwood, K., Gilchrest, B. A. Treatment
of children with port wine stains using the flashlamp-pulsed tunable dye
laser. N Engl J Med 1989; 320: 416 - 21.
-
Lanigan, S. W., Cotterill, J. A. Use of a lignocaine-prilocaine
cream as an analgesic in dye laser treatment of port wine stains. Lasers
Med Science 1987; 2: 87 - 89.
-
Renfro, L., Geronemus, R. G. Anatomical differences
of port-wine stains in response to treatment with the pulsed dye laser.
Arch Dermatol 1993; 129: 182 - 188.
-
Motley, R. J., Katugampola, G., Lanigan, S. W.,
Videomicroscopy of vascular patterns in port wine stains predicts outcome.
Lasers Surg Med 1996; Suppl 8: 94 - 99.
-
Lanigan, S. W., Port wine stains on the lower limb:
response to pulsed dye laser therapy. Clin Exp Dermatol 1996; 21:
88 - 92.
-
Swinehart, J. Hypertrophic scarring resulting
from flashlamp-pumped pulsed dye laser surgery. J Am Acad Dermatol
1991; 25: 845 - 46.
-
Glassberg, E., Lask, G., Rabinowitz, L. G.,
Tunnessen, W. W. Capillary haemangiomas: case study of a novel laser treatment
and a review of therapeutic options. J Dermatol Surg Oncol 1989;
15: 1214 - 1223.
-
Garden, J. M., Bakus, A. D., Paller, A. S. Treatment
of cutaneous haemangiomas by the flashlamp-pulsed dye laser: Prospective
analysis. J Pediatr 1992; 120: 555 - 60.
-
Barlow, R. J., Walker, N. P. J., Markey, A. C.,
Treatment of proliferative haemangiomas with the 585 nm pulsed dye laser.
Br J Dermatol 1996; 134: 700 - 704.
-
Varma, S., Lanigan, S. W. The psychological, social
and financial burden of tattoos. Br J Dermatol 1996; 135: Suppl
47: 37.
-
Lanigan, S. W., Sheehan-Dare, R. A., Cotterill,
J. A. The treatment of decorative tattoos with the carbon dioxide laser.
Br J Dermatol 1989; 120: 819 - 825.
-
Reid, W. H., Miller, I. D., Murphy, M. J., Paul, J.
P. and Evans, J. H. Q-Switched ruby laser treatment of tattoos, a 9-year
experience. Br J Plast Surg 1990; 43: 663 - 669.
-
Taylor, C. R., Gange, R. W., Dover, J. S. et al.
Treatment of tattoos by Q-Switched ruby laser. Arch Dermatol 1990;
126: 893 - 899.
-
Kilmer, S. L., Anderson, R. R. Clinical use of the
Q-Switched ruby and the Q-Switched Nd:YAG [1064 nm and 532 nm] lasers for
the treatment of tattoos. J Dermatol Surg Oncol 1993; 19: 330 -
338.
-
Taylor, C. R., Anderson, R. R., Gange, R. W. et
al. Light and electron microscope analysis of tattoos treated by Q-Switched
ruby laser. J Invest Dermatol 1991; 97: 131 - 6.
-
Lowe, N. J. Laser therapy of vascular benign pigmented
lesions and tattoos. In: Marks, R., Cunliffe, W. J. [eds], Skin Therapy.
London: Martin Dunitz, 1994.
-
Kilmer, S. L., Lee, M., Farinelli, W. et al. Q-Switched
Nd:YAG laser [1064 nm] effectively treats Q-Switched ruby laser resistant
tattoos. Lasers Surg Med 1992; Suppl. 4: 72.
-
Fitzpatrick, R. E. Comparison of the Q-Switched
ruby, Nd:YAG and alexandrite lasers in tattoo removal. Lasers Surg Med
1994; Suppl 6: 52.
-
Apfelberg, D. B., Maser, M. R., Lash, H., Rivers,
J. The argon laser for cutaneous lesions. JAMA 1981; 245: 2073 -
5.
-
Taylor, C. R., Flotte, T. J., Gange, W. R., Anderson,
R. R. Treatment of naevus of Ota by Q-Switched ruby laser. J Am Acad
Dermatol 1994; 30: 743 - 751.
-
Geronemus, R. G., Ashinoff, R. Use of the Q-Switched
ruby laser to treat tattoos and benign pigmented lesions of the skin. Lasers
Surg Med 1991; Suppl. 3, 64 - 5.
-
Ashinoff, R., Levine, V., Tse, Y., McClain, S.
Removal of pigmented lesions: comparison of the Q-Switched ruby and neodynium:
YAG lasers. Lasers Surg Med 1994; Suppl. 6: 50.
-
Kasai, K-I., Notodihardjo, H. W. Analysis of 200
nevus Ota patients who underwent Q-Switched Nd:YAG laser treatment. Lasers
Surg Med 1994; Suppl. 6: 50.
-
Goldberg, D. J., Stampien, T. Q-switched ruby
laser treatment of congenital naevi. Arch Dermatol 1995; 131: 621
- 623.
-
Waldorf, H. A., Kauvar, A. N. B., Geronemus, R.
G. Treatment of small and medium congenital naevi with the Q-switched ruby
laser. Arch Dermatol 1996; 132: 301 - 306.
-
Ruiz-Esparza, J., Fitzpatrick, R. E., Goldman,
M. P. Selective melanothermolysis: a histological study of the Candela
510 nm pulsed dye laser for pigmented lesions. Lasers Surg Med 1992;
Suppl. 4: 73.
-
Fitzpatrick, R. E., Goldman, M. P., Ruiz-Esparza,
J. Treatment of benign cutaneous pigmented lesions with the Candela 510
nm pulsed laser. Lasers Surg Med 1992; Suppl. 4: 73.
-
Reid, R. Physical and surgical principles governing
carbon dioxide laser surgery on the skin. Dermatol Clin 1991; 9:
297 - 316.
-
McBurney, E. I., Rosen, D. A. Carbon dioxide laser
treatment of verrucae vulgares. J Dermatol Surg Oncol 1984; 10:
45 - 8.
-
Street, M. L., Roenigk, R. K. Recalcitrant periungual
verrucae; the role of carbon dioxide laser vaporization. J Am Acad Dermatol
1990; 23: 115 - 20.
-
Apfelberg, D. B., Maser, M. R., Lash, H, et al.
Treatment of xanthelasma palpebrarum with carbon dioxide laser. J Dermatol
Surg Oncol 1987; 13: 149 - 51.
-
David, L. M. Laser vermilion ablation for actinic
cheilitis. J Dermatol Surg Oncol 1985; 11: 605 - 8.
-
Garden, J. M., O'Banion, M. K., Shelnitz, L. S.
et al. Papillomavirus in the vapor of carbon dioxide laser-treated verrucae.
JAMA 1988; 259: 1199 - 202.
-
Hruza, G. J. and Dover, J. S. Laser skin resurfacing.
Arch Dermatol 1996; 32: 451 - 458.
-
Wheeland, R. G. Clinical uses of lasers in dermatology.
Lasers Surg Med 1995; 16[1]: 2 - 23.
-
Gardner, E. S., Reinisch, L., Stricklin, G. P.
and Ellis, D. L. In vitro changes in non-facial human skin following CO2
laser resurfacing. Lasers Surg Med 1996; 19: 379 - 387.
Resources
All materials
copyright © 1992-Feb 2001 by SMTL, March 2001 et seq by SMTL
unless otherwise stated.
|
Home |
Index |
Subject Areas |
SMTL |
Site Map |
Archive |
Contact Us
|
http://www.worldwidewounds.com/1997/july/Lanigan/Lanigan-1.0.html
Last Modified: Tuesday, 11-Dec-2001 11:40:09 GMT



 click on image for full size illustration
click on image for full size illustration
 click on image for full size illustration
click on image for full size illustration
 Click on image for full size illustration
Click on image for full size illustration

 click on image for full size illustration
click on image for full size illustration